Quick Links
- Can a corneal ulcer heal on its own?
- Symptoms of a Corneal Ulcer
- What Causes a Corneal Ulcer?
- Risk Factors for Corneal Ulcer
- Why a Corneal Ulcer Is an Emergency
- Diagnosis of Corneal Ulcer
- Corneal Ulcer Treatment Options
- Types of Corneal Transplant Procedures
- When Is a Corneal Transplant Necessary?
- Recovery After Corneal Transplant
- Outlook and Prognosis
- Preventing Corneal Ulcers
- When to Seek Immediate Care
- Great External Resources
- Frequently Asked Questions (FAQs)
What Is a Corneal Ulcer?
A corneal ulcer is a wound in the corneal tissue, often resulting from infection, trauma, severe dry eye, or improper contact lens use. Because the cornea plays a critical role in focusing light onto the retina, any damage to it can significantly affect vision.
The cornea also acts as a protective barrier against bacteria, viruses, fungi, and parasites. When this barrier is disrupted — even by a small scratch — harmful microorganisms can penetrate the surface and cause a serious infection known as infectious keratitis. If untreated, this infection can progress into a corneal ulcer.
Corneal ulcers are considered a medical emergency. Early treatment dramatically improves outcomes and reduces the risk of complications.
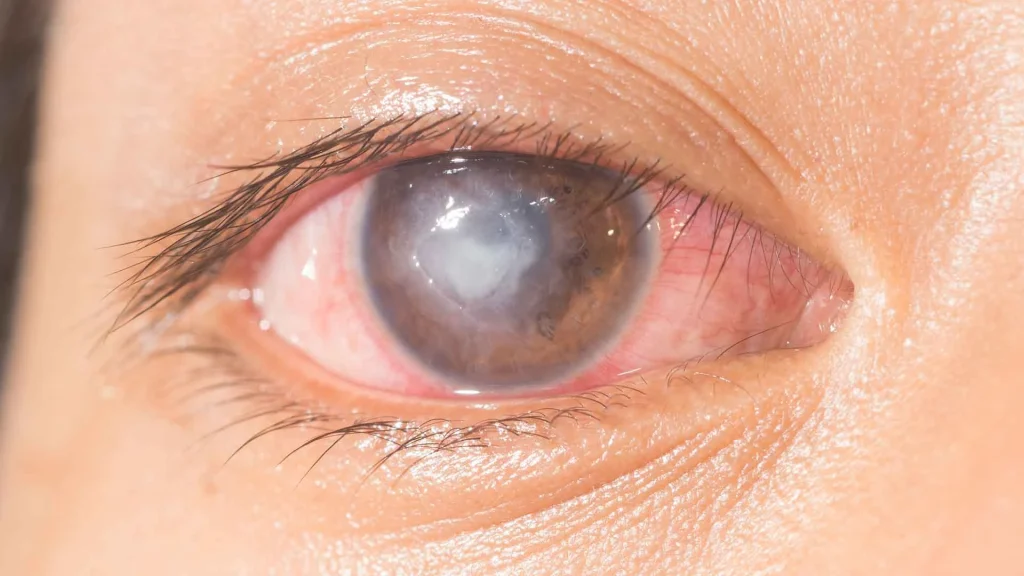
Symptoms of a Corneal Ulcer
Symptoms can develop quickly and may worsen within hours or days. Common signs include:
Severe eye pain
Redness or bloodshot appearance
Blurred or decreased vision
Sensitivity to light (photophobia)
Excessive tearing
Eye discharge (pus or mucus)
Swelling of the eyelids
A visible white or gray spot on the cornea
Feeling like something is stuck in the eye
If you experience sudden eye pain or vision changes, immediate evaluation is critical.
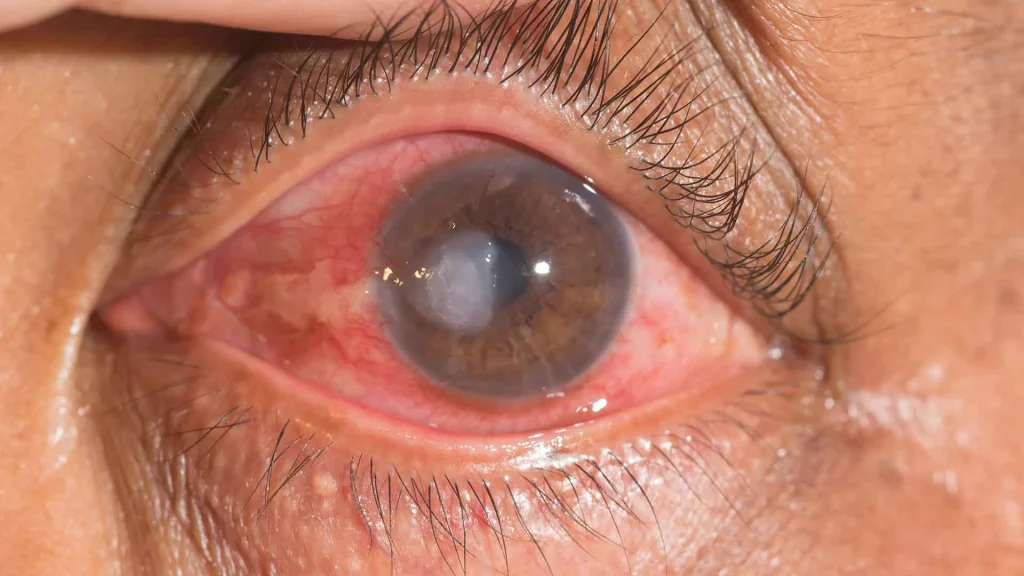
What Causes a Corneal Ulcer?
Corneal ulcers are typically divided into infectious and noninfectious causes.
Infectious Causes
Infections are the most common cause of corneal ulcers and can include:
Bacterial Infections
Often linked to contact lens wear, especially overnight use. Bacteria can enter through tiny scratches in the cornea and multiply rapidly.
Viral Infections
Herpes simplex virus is a leading viral cause. These ulcers may recur and require specialized treatment.
Fungal Infections
More common after eye injuries involving plant material or soil exposure. These infections tend to progress slowly but can be severe.
Parasitic Infections
Acanthamoeba infections are rare but serious and often associated with swimming while wearing contact lenses or improper lens hygiene.
Noninfectious Causes
Not all corneal ulcers result from infection. Other causes include:
Eye trauma or chemical burns
Severe dry eye disease
Inability to fully close the eyelids
Autoimmune disorders
Improper use of steroid eye drops
Regardless of cause, untreated corneal ulcers can lead to permanent damage.
Risk Factors for Corneal Ulcer
Certain individuals are at higher risk of developing a corneal ulcer:
Contact lens wearers (especially overnight use)
Poor contact lens hygiene
History of herpes eye infections
Dry eye syndrome
Autoimmune conditions
Diabetes
Recent eye injury or surgery
Use of steroid eye drops
Contact lens wear remains the leading preventable risk factor.
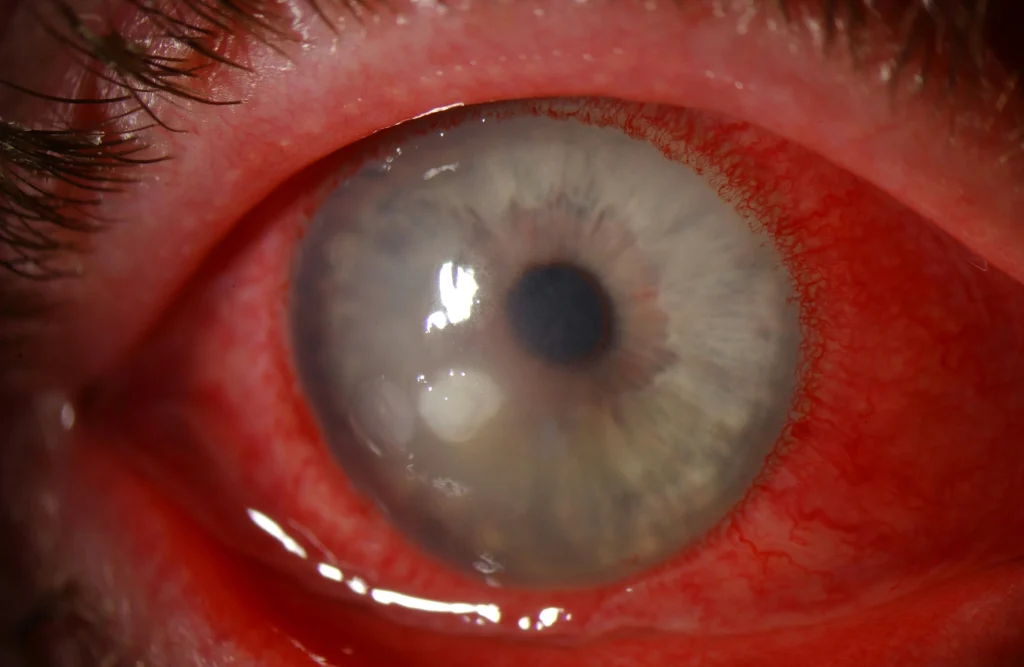
Why a Corneal Ulcer Is an Emergency
The cornea has no blood vessels, meaning it relies on surrounding tissues and tears for nutrients and immune defense. Once infected, damage can spread quickly.
Delays in treatment increase the risk of:
Corneal scarring
Corneal thinning or perforation
Endophthalmitis (severe internal eye infection)
Glaucoma
Cataracts
Permanent vision loss
Need for corneal transplant
Prompt diagnosis and aggressive treatment can prevent these complications.
Diagnosis of Corneal Ulcer
Accurate diagnosis is essential to determine the cause and appropriate treatment.
Comprehensive Eye Examination
Our specialists perform:
Visual acuity testing
Slit-lamp examination for detailed corneal evaluation
Fluorescein staining to highlight damaged areas
Intraocular pressure assessment (if safe)
Corneal Culture and Laboratory Testing
In moderate to severe cases, a small corneal sample may be collected to identify the specific microorganism responsible. This allows for targeted therapy.
Early identification of the infection type improves treatment success and reduces complications.
Corneal Ulcer Treatment Options
Treatment depends on the underlying cause, severity, and depth of the ulcer.
1. Antibiotic Eye Drops (Bacterial Ulcers)
For bacterial corneal ulcers, intensive antibiotic drops are the first line of treatment. Drops may be administered every hour initially. In severe cases, oral or intravenous antibiotics may be required.
Hospitalization may be recommended for large or central ulcers.
2. Antiviral Therapy (Viral Ulcers)
Herpes-related corneal ulcers are treated with antiviral eye drops or oral medications. Steroids may be used carefully under close supervision once infection control is established.
3. Antifungal Therapy (Fungal Ulcers)
Fungal ulcers require specialized antifungal drops and sometimes oral medications. These infections often require longer treatment durations.
4. Treatment for Parasitic Ulcers
Acanthamoeba infections require prolonged therapy using anti-parasitic medications. Early diagnosis significantly improves outcomes.
5. Supportive Treatments
Additional supportive measures may include:
Pain control medications
Cycloplegic drops to reduce inflammation
Protective bandage contact lenses
Temporary eyelid closure procedures (tarsorrhaphy) in severe exposure cases
Types of Corneal Transplant Procedures
Depending on the depth of corneal damage, different transplant techniques may be used.
Partial Thickness (Lamellar) Transplant
Only the damaged layers are replaced, preserving healthy tissue. This approach often results in faster recovery and lower rejection risk.
Full Thickness Transplant (Penetrating Keratoplasty)
The entire cornea is replaced when damage is extensive.
Your eye specialist will determine the most appropriate approach based on your specific condition.
When Is a Corneal Transplant Necessary?
Despite aggressive medical treatment, some corneal ulcers result in significant scarring, thinning, or perforation. In these cases, a corneal transplant may be required.
A corneal transplant replaces damaged corneal tissue with healthy donor tissue. This procedure can:
Restore clarity
Repair structural damage
Prevent eye rupture
Improve visual function
Corneal transplant surgery is typically recommended when:
The ulcer has caused severe scarring
The cornea has perforated
Infection does not respond to medication
Vision is significantly impaired
Modern corneal transplant techniques have high success rates, especially when performed promptly.
Recovery After Corneal Transplant
Recovery from a corneal transplant requires careful monitoring.
Postoperative care includes:
Antibiotic and anti-inflammatory eye drops
Regular follow-up visits
Activity restrictions
Monitoring for signs of rejection
Vision improvement may take several months as healing progresses.
With proper care, many patients regain functional vision and significantly improved quality of life.
Outlook and Prognosis
The prognosis of a corneal ulcer depends on:
Size and location of the ulcer
Type of infection
Speed of diagnosis
Response to treatment
Overall eye health
Small, superficial ulcers treated early often heal with minimal scarring. Larger or central ulcers may affect vision permanently.
When corneal transplant is required, outcomes are generally favorable, especially when infection has been controlled.
Preventing Corneal Ulcers
While not all corneal ulcers can be prevented, risk can be significantly reduced through proper eye care.
Contact Lens Safety
- Never sleep in contact lenses unless approved
- Replace lenses as recommended
- Use sterile cleaning solution only
- Never use tap water to clean lenses
- Avoid swimming or showering with lenses
- Wash hands before handling lenses
Protect Your Eyes
- Wear protective eyewear during risky activities
- Avoid rubbing your eyes
- Treat dry eye conditions promptly
- Manage autoimmune diseases carefully
Early care prevents complications.
When to Seek Immediate Care
Contact an eye specialist immediately if you experience:
Sudden eye pain
Vision changes
Increasing redness
Light sensitivity
Eye discharge
Worsening symptoms despite treatment
Delaying care can increase the risk of permanent damage.
Great External Resources
Frequently Asked Questions (FAQs)
When to do eye cataract surgery?
A corneal ulcer is an open sore on the cornea, usually caused by infection, injury, or underlying eye conditions. While minor abrasions on the cornea may heal naturally, most corneal ulcers cannot heal on their own. Left untreated, they can worsen quickly, leading to serious complications such as scarring, vision loss, or even blindness. Prompt medical evaluation is essential to determine the cause and start the right treatment, which may include antibiotic, antifungal, or antiviral eye drops. Self-healing is rare, and relying on it can put your vision at risk.
Can a corneal ulcer lead to blindness?
Yes, a corneal ulcer can potentially lead to blindness if it is severe or left untreated. The cornea is crucial for focusing light onto the retina, and damage from an ulcer can cause scarring or perforation, disrupting vision permanently. Rapid and effective treatment is essential to prevent permanent vision loss. Early intervention with medications, protective contact lenses, or surgery can save vision in many cases. Regular follow-ups are also important to monitor healing and prevent complications. Ignoring symptoms like pain, redness, or blurred vision can increase the risk of serious, irreversible damage.
Can a corneal ulcer be cured?
Yes, a corneal ulcer can often be cured if treated promptly and appropriately. Treatment depends on the cause—bacterial, fungal, viral, or traumatic. Doctors usually prescribe medicated eye drops, oral medications, or, in severe cases, surgical interventions such as corneal transplantation. The key is early diagnosis and strict adherence to treatment, as delayed care can lead to permanent scarring or vision loss. In addition to medications, patients may be advised to avoid contact lenses, maintain eye hygiene, and attend follow-up appointments. Timely treatment significantly increases the likelihood of full recovery without lasting vision problems.
Can a corneal ulcer be treated?
Absolutely, corneal ulcers can be treated effectively with medical care. The treatment plan depends on the underlying cause. Bacterial ulcers usually require antibiotic drops, while fungal ulcers need antifungal medications. Viral ulcers may require antiviral therapy. Pain and inflammation are often managed with protective eye drops or ointments. In severe cases, surgical intervention such as a corneal transplant may be necessary. Early treatment is critical to prevent complications such as scarring or perforation, which can permanently impair vision. Regular monitoring by an eye specialist ensures proper healing and reduces the risk of recurrence.
Can a corneal ulcer spread to the other eye?
The ulcer itself does not typically spread directly from one eye to the other. However, the underlying cause, such as viral infections (like herpes simplex) or bacterial contamination, can affect both eyes if hygiene precautions are not taken. Sharing towels, eye drops, or rubbing the eyes can increase the risk of spreading the infection. It’s essential to follow strict eye hygiene, use medications as prescribed, and avoid contact with others’ eyes. Preventive measures and prompt treatment can significantly reduce the likelihood of the second eye being affected.
Can a corneal ulcer cause headaches?
Yes, it can sometimes lead to headaches, though indirectly. The ulcer causes intense eye pain, irritation, and photophobia (sensitivity to light), which can trigger tension headaches or migraines. Persistent discomfort and squinting can strain the surrounding muscles, leading to head pain. Treating the corneal ulcer effectively usually alleviates these secondary headaches. If you experience severe headache alongside eye pain, it’s important to consult an eye specialist immediately to rule out complications such as infection spreading deeper into the eye or other neurological issues.
What does a corneal ulcer feel like?
They usually causes sharp eye pain, redness, tearing, and a feeling of something being stuck in the eye. Patients often experience blurred vision, sensitivity to light, and sometimes discharge. The discomfort may worsen when blinking or exposing the eyes to sunlight. Severe ulcers can cause intense pain that interferes with daily activities. Because the cornea has a high density of nerve endings, even small ulcers can be extremely painful. Early evaluation by an ophthalmologist is essential to reduce pain, treat the infection, and prevent long-term vision damage.
What causes a corneal ulcer?
They can be caused by several factors: bacterial, viral, fungal, or parasitic infections, eye injuries, dry eyes, contact lens misuse, or underlying eye conditions. Trauma to the cornea, like scratches or chemical burns, can create an entry point for infection. Poor contact lens hygiene is a common cause, as it allows bacteria or fungi to thrive on the corneal surface. Immune disorders or chronic eye diseases can also increase susceptibility. Identifying the underlying cause is critical for effective treatment, as the management strategy differs based on whether the ulcer is infectious or non-infectious.
How long does a corneal ulcer take to heal?
The healing time depends on its severity, size, and cause. Minor ulcers may heal within 1–2 weeks, while more severe or deep ulcers can take several weeks or even months. Healing is also influenced by how quickly treatment begins and patient compliance with medications. Fungal or viral ulcers often take longer to resolve than bacterial ulcers. Regular follow-ups with an eye specialist are crucial to monitor progress and prevent complications like scarring. Neglecting treatment can prolong healing and increase the risk of permanent vision impairment.
How to cure a corneal ulcer?
Curing it involves prompt and appropriate medical intervention. The first step is visiting an ophthalmologist to identify the cause. Treatment usually includes antibiotic, antifungal, or antiviral eye drops, pain-relief medications, and sometimes steroid drops to reduce inflammation. Severe ulcers may require surgical procedures, including debridement or corneal transplantation. Good eye hygiene, avoiding contact lenses during recovery, and regular follow-ups are crucial to ensure full healing. Early treatment significantly improves outcomes and reduces the risk of scarring, vision loss, or recurrence. Never attempt home remedies, as they can worsen the condition.