Quick Links
- What Is a Chalazion?
- Causes of Chalazion
- Symptoms of a Chalazion Eye
- Diagnosis of Chalazion
- Chalazion Treatment Options
- Prevention of Chalazion
- Living With Chalazion
- Complications of Chalazion Eye
- Chalazion vs. Stye
- Risk Factors for Recurrent Chalazia
- The Role of Meibomian Gland Dysfunction (MGD)
- When Imaging or Biopsy Is Considered
- Recovery After Chalazion Removal
- Chalazion in Children
- Impact on Vision and Corneal Shape
- Lifestyle Adjustments to Support Eyelid Health
- Psychological and Cosmetic Considerations
- When to Seek Urgent Care
- Great External Resources
- Frequently Asked Questions (FAQs)
What Is a Chalazion?
A chalazion is a swelling of the eyelid caused by blockage of an oil gland, medically known as a meibomian gland. These glands produce an oily substance that helps lubricate the eye. When the gland becomes clogged, the trapped oil can form a firm, painless lump on the eyelid.
Typically, a chalazion develops on the upper eyelid but can occasionally occur on the lower lid. While anyone can develop a chalazion, adults aged 30–50 are most commonly affected. Children can develop chalazia as well, though it is less frequent.
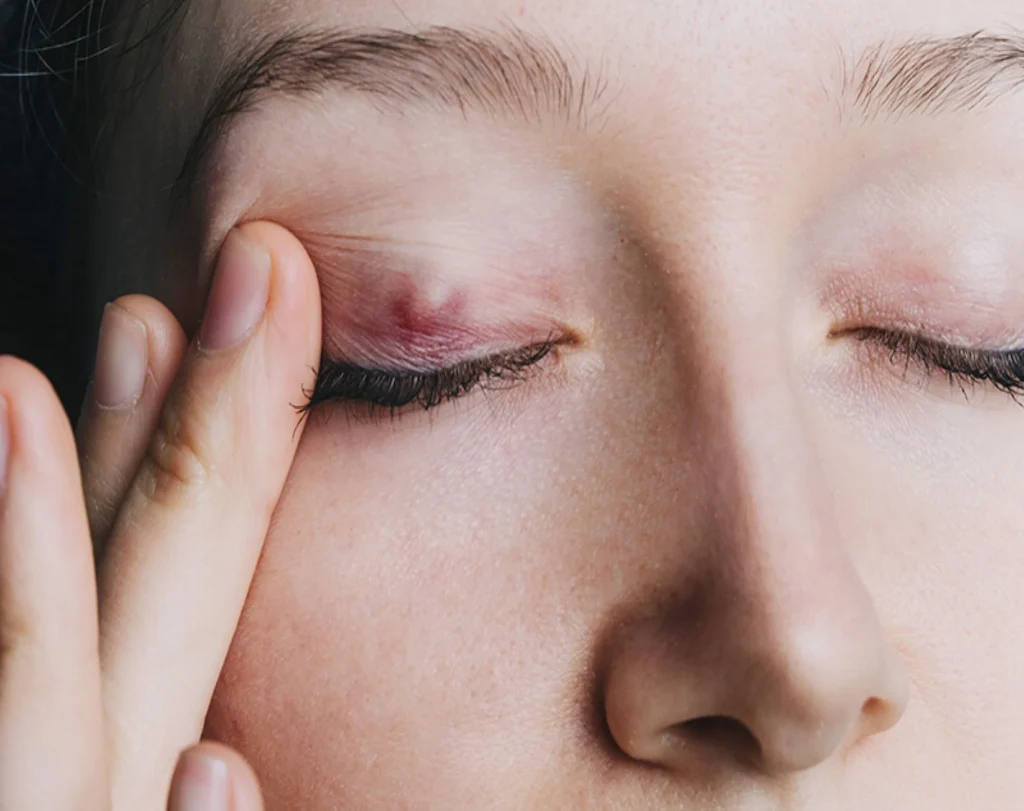
Causes of Chalazion
A chalazion develops when an oil-producing gland becomes blocked. Several factors can contribute to this:
Chronic blepharitis: Inflammation of the eyelid can increase the likelihood of gland blockages.
Skin conditions: Conditions such as acne rosacea or seborrheic dermatitis can make the eyelids more prone to blockages.
Hormonal changes: Fluctuations in hormones may affect gland function.
Previous chalazia: Individuals who have had a chalazion before are at higher risk for recurrence.
Dry eyes: Lack of proper lubrication can increase the risk of gland obstruction.
Rarely, persistent chalazia can indicate other underlying issues, including infections or, in very uncommon cases, skin cancers.
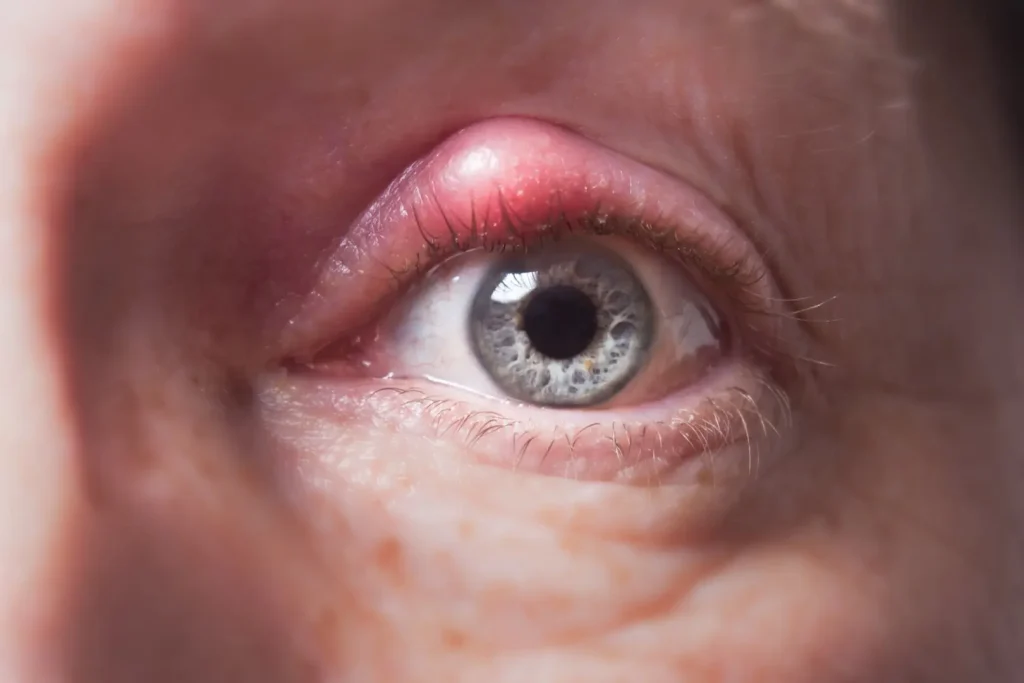
Symptoms of a Chalazion Eye
Their can vary depending on its size and location:
Small, painless bump on the eyelid
Redness or mild tenderness
Mild irritation causing tearing or scratchy sensations in the eye
Blurred vision if they grow large enough to press on the eyeball
Occasionally, swelling of the entire eyelid if they becomes particularly large
They may initially resemble a stye but usually becomes less tender as they develops. It is important to monitor the lesion and seek professional care if it persists or affects vision.
Diagnosis of Chalazion
Diagnosing a chalazion is generally straightforward for an eye care professional. The process typically involves:
Patient history: Understanding previous eye issues, skin conditions, and general health helps determine contributing factors.
External eye exam: Inspection of the eyelid, eyelashes, and surrounding skin for abnormalities.
Eyelid examination: Using magnification and bright light, the oil gland openings on the underside of the eyelid are evaluated.
Occasionally, if a chalazion persists or has atypical features, further testing may be recommended to rule out other conditions.

Chalazion Treatment Options
Most chalazia resolve on their own within a few weeks, but chalazion treatment can speed recovery and prevent recurrence. Treatment depends on the size, severity, and frequency of the chalazion.
Home Care
For small, uncomplicated chalazia, home care is often sufficient:
Warm compresses: Apply a clean, warm cloth to the affected eyelid for 10–15 minutes, 3–6 times daily. This helps soften the hardened oil blocking the gland and promotes drainage.
Gentle massage: Carefully massaging the eyelid can help the gland clear itself.
Hygiene practices: Avoid touching the eyes, and ensure proper cleaning of eyelids. Discontinue eye makeup while the chalazion heals.
Avoid popping or squeezing: Attempting to pop a chalazion can increase irritation or risk of infection.
With diligent care, many chalazia heal within a few weeks without medical intervention.
Medical Treatments
If a chalazion persists beyond several weeks, professional intervention may be necessary:
Steroid injections: Reduce inflammation and swelling, particularly for larger chalazia.
Incision and drainage: A minor surgical procedure performed under local anesthesia to remove the blocked contents of the chalazion.
Antibiotics: Usually reserved for cases with secondary bacterial infection or styes that precede chalazion formation.
Chalazion removal is typically quick, minimally invasive, and highly effective, though it is reserved for chalazia that do not respond to conservative management.
Prevention of Chalazion
Preventing chalazia often focuses on maintaining good eyelid hygiene and managing underlying conditions:
Wash hands before touching your eyes or contact lenses.
Clean eyelids daily to remove dirt, makeup, and debris.
Remove eye makeup before bed and replace mascara, eyeliner, and eye shadow every 2–3 months.
Consider eyelid scrubs with mild baby shampoo or commercially available lid cleansers, particularly if you have blepharitis.
Manage skin conditions such as rosacea or seborrheic dermatitis, which may increase risk.
Practicing these habits reduces the chance of chalazion recurrence and supports overall eye health.
Living With Chalazion
Most chalazia are benign and resolve on their own, but there are situations when you should seek professional attention:
The chalazion does not improve after several weeks of home care.
Vision becomes blurred due to pressure from the chalazion.
Recurring chalazia suggest underlying eyelid inflammation or other eye conditions.
There is unexpected redness, pain, or discharge, which may indicate infection.
During a consultation, it is helpful to ask your eye care provider about:
The expected timeline for healing
Treatment options for faster recovery
Preventive strategies for future chalazia
Complications of Chalazion Eye
While rare, complications can occur if it is left untreated:
Visual disturbances: Large chalazia pressing on the cornea may cause temporary blurred vision.
Recurrent chalazia: Frequent formation may indicate chronic eyelid issues such as blepharitis.
Secondary infection: Though uncommon, a blocked gland can become infected, leading to pain and redness.
Prompt and appropriate treatment minimizes these risks.
Chalazion vs. Stye: Understanding the Difference
Although chalazia and styes are often confused, they are not the same condition. A stye (hordeolum) is typically caused by a bacterial infection of an eyelash follicle or oil gland and is usually painful, red, and swollen. It often develops quickly and may produce pus.
A chalazion, on the other hand, is primarily caused by gland blockage rather than infection. It tends to grow more slowly and is usually painless after the initial inflammation subsides. While a stye can sometimes turn into a chalazion if inflammation blocks the gland, proper diagnosis helps determine the most appropriate treatment approach.
Understanding the distinction ensures that the correct management plan is followed and prevents unnecessary use of antibiotics when they are not needed.
Risk Factors for Recurrent Chalazia
Some individuals are more prone to developing repeated chalazia. Chronic eyelid inflammation is one of the most significant contributing factors. Conditions affecting oil production and skin health can disrupt the normal flow of the meibomian glands.
Risk factors may include:
Meibomian gland dysfunction (MGD)
Oily skin types
Long-term contact lens use
Inadequate eyelid hygiene
High screen time leading to reduced blinking
Environmental irritants such as smoke or pollution
Digital device use, in particular, has become a modern contributor. Reduced blink rates during prolonged screen time may prevent proper oil distribution across the tear film, increasing the likelihood of gland blockage.
Identifying and managing these risk factors can significantly lower recurrence rates.
The Role of Meibomian Gland Dysfunction (MGD)
Meibomian gland dysfunction is a common underlying cause of their formation. The meibomian glands line the edges of the eyelids and secrete oils that prevent tears from evaporating too quickly. When these glands become clogged or produce poor-quality oil, inflammation and blockage can occur.
MGD is often associated with:
Dry eye syndrome
Aging
Hormonal fluctuations
Inflammatory skin disorders
Managing MGD may involve specialized treatments such as thermal pulsation therapy, prescription medications, or in-office gland expression. Addressing gland dysfunction not only helps treat chalazia but also improves overall tear stability and comfort.
When Imaging or Biopsy Is Considered
In rare cases, additional evaluation may be necessary. If a lesion repeatedly appears in the same location, does not respond to standard treatment, or has unusual characteristics (such as lash loss or irregular borders), further investigation may be recommended.
This can include:
Slit-lamp examination for detailed evaluation
Imaging in atypical cases
Biopsy to rule out rare eyelid tumors
While the vast majority of chalazia are benign, persistent or atypical lesions should always be examined carefully to ensure accurate diagnosis.
Recovery After Chalazion Removal
After minor surgical removal, recovery is typically straightforward. Mild swelling or bruising may occur for several days. Patients are often advised to:
Use prescribed antibiotic or anti-inflammatory ointment
Avoid heavy eye makeup for at least one week
Refrain from strenuous activity for a short period
Continue gentle warm compresses if recommended
Most individuals resume normal activities within 24–48 hours. Visible scarring is uncommon because the incision is usually made on the inner surface of the eyelid.
Chalazion in Children
Although less common, children can develop chalazia. Young patients may rub their eyes frequently due to allergies or irritation, increasing the likelihood of gland blockage.
Management in children typically focuses on:
Warm compresses with parental supervision
Gentle lid hygiene
Monitoring for changes in size or symptoms
In persistent cases, treatment may require specialist evaluation. Early management helps prevent discomfort and minimizes the risk of visual interference during developmental years.
Impact on Vision and Corneal Shape
Large chalazia can temporarily affect the curvature of the cornea by exerting pressure on the surface of the eye. This may lead to mild astigmatism, causing blurred or distorted vision.
Importantly, these changes are usually reversible once they resolve or are removed. Prompt treatment prevents prolonged corneal distortion and ensures visual clarity is restored.
Lifestyle Adjustments to Support Eyelid Health
Supporting long-term eyelid health can significantly reduce recurrence. In addition to hygiene practices, consider:
Taking regular breaks during screen use (20-20-20 rule)
Increasing omega-3 intake to support oil gland function
Staying hydrated
Using preservative-free artificial tears if dryness is present
Avoiding expired or low-quality eye cosmetics
For individuals prone to chronic eyelid inflammation, routine maintenance may be necessary even when they are present.
Psychological and Cosmetic Considerations
While chalazia are medically benign, they can cause cosmetic concern. A visible eyelid lump may affect confidence, especially in professional or social settings. Understanding that chalazia are common and treatable can ease anxiety.
When necessary, timely medical management provides both functional and cosmetic improvement, helping patients feel comfortable in daily interactions.
When to Seek Urgent Care
Although most chalazia are harmless, immediate medical attention should be sought if you experience:
Rapidly increasing swelling
Severe pain
Fever
Spreading redness
Significant vision changes
These symptoms may indicate infection or another condition requiring prompt treatment.
Great External Resources
Frequently Asked Questions (FAQs)
Why do chalazions happen?
They happen when one of the small oil glands (meibomian glands) in the eyelid becomes blocked. The trapped oil builds up inside the gland, causing swelling and forming a firm lump on the eyelid.
How is a chalazion caused?
They are caused by blockage of an oil-producing gland in the eyelid. Factors such as blepharitis (eyelid inflammation), rosacea, dry skin, hormonal changes, or previous styes can increase the risk of gland blockage.
Can a chalazion spread?
No, they cannot spread from one person to another because it is not an infection. It is caused by a blocked gland, not bacteria. However, a person who is prone to chalazions may develop more than one over time.
Can a chalazion heal on its own?
Yes, many heal on their own within a few weeks. Warm compresses and good eyelid hygiene can help speed up the healing process.
Can a chalazion cause blurry vision?
Yes, if they become large enough, it can press against the eyeball and temporarily cause blurry vision. Once the swelling reduces or the chalazion is treated, vision usually returns to normal.
Can a chalazion be painful?
They are usually painless. However, it may be tender or slightly painful in the early stages. If significant pain develops, it could indicate infection or a stye.
How is a chalazion removed?
Removal involves a small incision made on the inside of the eyelid to drain the blocked oil and reduce swelling. In some cases, a steroid injection may be used instead to shrink the lump.
Can a chalazion come and go?
Yes, some may shrink and then return, especially if underlying conditions like blepharitis or rosacea are not managed. Practicing proper eyelid hygiene can reduce recurrence.
Can a chalazion lead to cancer?
In most cases, they are completely benign and not cancerous. However, if a chalazion does not heal, keeps recurring in the same location, or looks unusual, an eye specialist may recommend further evaluation to rule out rare conditions.
How does a chalazion cause astigmatism?
A large one can press against the surface of the eye (the cornea), temporarily changing its shape. When the cornea becomes slightly distorted, light does not focus evenly, which can result in temporary astigmatism and blurred vision.
This effect usually resolves once they shrink or are removed.
Will a chalazion come to a head?
Unlike a stye, a chalazion does not typically “come to a head.” They are caused by a blocked oil gland rather than an active bacterial infection, so they usually form a firm, rounded lump instead of a pus-filled point.
If a lesion develops a visible yellow spot or drains pus, it may actually be a stye or a chalazion that has become secondarily infected.
Will a chalazion burst?
In some cases, they may drain on their own. When this happens, it may release oily or thick material rather than pus. However, many chalazia slowly shrink without bursting.
It is important not to squeeze or pop them, as this can worsen inflammation or lead to infection.
Which bacteria causes a chalazion?
They are not primarily caused by bacteria. It develops due to blockage of a meibomian (oil) gland.
However, styes — which can sometimes lead to their formation — are commonly caused by Staphylococcus bacteria. If a chalazion becomes infected, bacteria may be involved secondarily.