Quick Links
- What is abnormal head posture?
- What is ocular torticollis?
- Preventing Strain and Supporting Healthy Visual Alignment
- Causes of Abnormal Head Posture
- Non-ocular causes
- Symptoms and Indicators
- Why Early Evaluation Matters
- Diagnostic Assessment
- Additional testing
- Differentiation of causes
- Treatment Options
- Pediatric Considerations
- Living with Abnormal Head Posture
- Outlook and Long-Term Results
- Great External Resources
- Frequently Asked Questions (FAQs)
What is abnormal head posture?
Abnormal head posture describes any situation in which the head is not held in a neutral, straight position during visual focus. It may appear as:
Tilting the head to one side
Turning the face left or right
Raising or lowering the chin
Combining several of these movements
This positioning often develops subconsciously as a way to improve vision or reduce discomfort.
When the posture arises from visual causes, it is commonly referred to as ocular torticollis. This type of adaptation helps maintain clearer or more stable vision but indicates that an underlying condition should be addressed.
What is ocular torticollis?
Ocular torticollis is a compensatory head posture adopted to optimize visual performance. Rather than being the primary disorder, it reflects an adjustment made by the visual system in response to eye-related challenges.
Individuals may adjust their head position to:
Achieve better eye alignment
Reduce double vision
Improve focus
Stabilize visual perception
Although it often appears early in life, ocular torticollis can develop at any age and may become more pronounced if untreated.
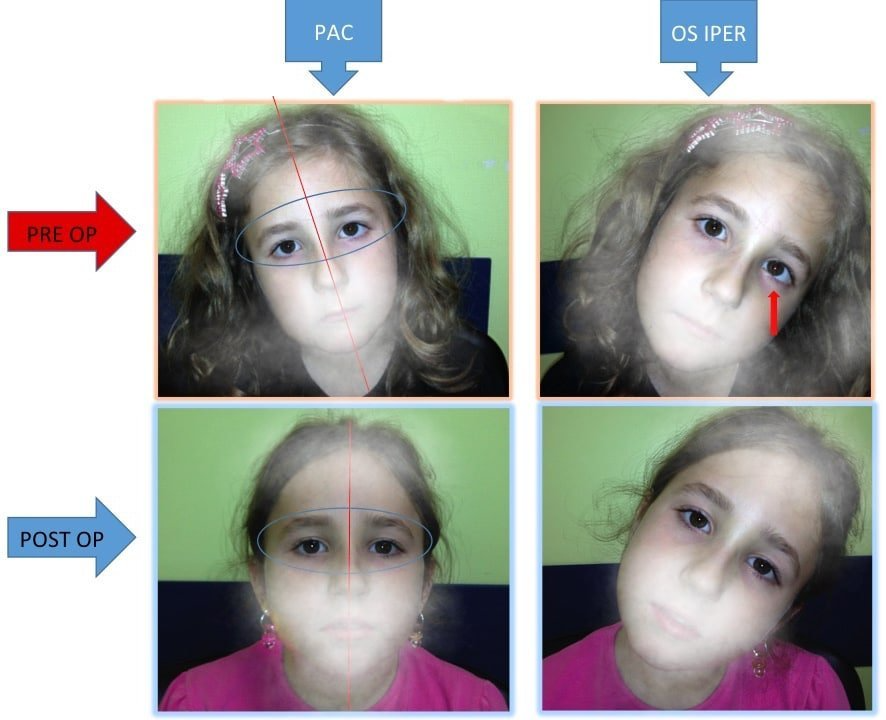
Preventing Strain and Supporting Healthy Visual Alignment
While not all causes of abnormal head posture or ocular torticollis can be prevented, certain habits and proactive steps can support long-term visual comfort and reduce unnecessary strain.
Maintain regular visual monitoring
Routine eye assessments help identify changes in alignment, focusing ability, or coordination early. Detecting issues before compensatory posture develops can reduce the likelihood of long-term discomfort.
Optimize visual environments
Daily surroundings play an important role in posture habits. Consider:
Keeping screens at eye level
Maintaining proper lighting to avoid visual strain
Sitting at appropriate viewing distances
Taking regular breaks during prolonged focus tasks
These adjustments encourage natural head positioning and visual efficiency.
Encourage balanced posture habits
Promoting awareness of body alignment supports both visual and musculoskeletal health:
Avoid prolonged tilting or leaning positions
Use ergonomic seating when possible
Support upright head alignment during reading or device use
Incorporate stretching routines for the neck and shoulders
Monitor developmental changes in children
Young individuals may not notice or communicate posture issues. Caregivers should watch for:
Consistent head tilt during viewing
Closing one eye while focusing
Frequent repositioning when reading or watching screens
Complaints of headaches or discomfort
Early attention supports healthy visual development.
Causes of Abnormal Head Posture
Determining the cause is essential because treatment targets the underlying condition rather than the posture itself.
Eye misalignment
When the eyes are not properly aligned, turning or tilting the head can reduce visual conflict and improve coordination between the eyes.
Eye misalignment
When the eyes are not properly aligned, turning or tilting the head can reduce visual conflict and improve coordination between the eyes.
Involuntary eye movement
Conditions involving unstable eye motion may lead individuals to find head positions that enhance visual clarity.
Unequal vision between eyes
Differences in visual strength may cause head positioning that favors the stronger eye.
Eyelid obstruction
A drooping eyelid may prompt adjustments in chin or head angle to maintain a clear field of view.
Uncorrected refractive issues
Blurred vision due to focusing problems can sometimes lead to compensatory posture.

Non-ocular causes
Not all cases are related to vision. Other potential contributors include:
Tight neck muscles
Structural skeletal differences
Neurological factors
Hearing imbalance
Musculoskeletal injury
A comprehensive assessment ensures the true source is identified.
Symptoms and Indicators
Abnormal head posture can vary widely in presentation. Common signs include:
Persistent head tilt or turn
Visual discomfort or strain
Double vision
Frequent headaches
Neck tension or pain
Difficulty focusing
Changes in facial symmetry over time
Children may not report symptoms because the posture improves their vision, making observation important.
Why Early Evaluation Matters
Ignoring abnormal head posture may allow complications to develop.
Physical discomfort
Long-term positioning can lead to muscle strain and chronic pain.
Skeletal and facial changes
Persistent tilt during growth may influence structural development.
Reduced visual efficiency
Untreated visual causes may worsen or limit performance in daily tasks.
Developmental impact
In younger individuals, uncorrected issues may affect learning or coordination.
Early intervention helps reduce these risks.
Diagnostic Assessment
Assessment generally includes:
Medical and visual history review
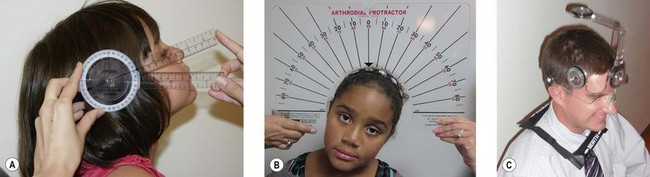
Observation of head positioning
Measurement of tilt or rotation
Vision and alignment testing
These steps help determine patterns and triggers.
Additional testing
Depending on findings, further evaluation may involve:
Eye movement tracking
Binocular coordination tests
Refraction measurements
Retinal and internal eye examination
Occlusion testing
These help clarify whether posture changes are vision-related.
Differentiation of causes
Because origins may vary, evaluation may involve additional screening to distinguish between visual, neurological, or musculoskeletal factors. This ensures accurate treatment planning.
Treatment Options
Management depends on diagnosis and severity.
Vision-focused approaches
Corrective lenses
Addressing focusing issues can reduce compensatory positioning.
Visual therapy techniques
Exercises or structured programs may improve coordination between the eyes.
Occlusion methods
Temporary patching may help strengthen weaker visual pathways.
Surgical options
In certain cases, procedures may be considered to:
Improve eye alignment
Reduce visual imbalance
Enhance binocular coordination
These interventions aim to restore natural head positioning and comfort.
Physical rehabilitation
If posture is related to muscular factors:
Stretching routines
Strengthening exercises
Postural retraining
may provide improvement.
Integrated management
Some individuals benefit from combining multiple approaches, ensuring both visual and physical contributors are addressed.
Pediatric Considerations
Children often adapt quickly to visual challenges, making abnormal head posture less obvious. Important considerations include:
Early monitoring of visual development
Regular evaluations
Addressing underlying causes promptly
Supporting balanced growth and coordination
Timely care can significantly improve developmental outcomes.
Living with Abnormal Head Posture
Daily care strategies
Follow prescribed corrective measures
Maintain posture awareness
Attend scheduled evaluations
Monitor symptom changes
Lifestyle adjustments
Ergonomic setups, proper screen placement, and supportive routines can reduce strain and encourage natural alignment.
Outlook and Long-Term Results
With accurate diagnosis and targeted treatment:
Visual comfort often improves
Head posture normalizes
Physical strain decreases
Daily performance enhances
Outcomes depend on cause, duration, and responsiveness to intervention, but early attention generally leads to better results.
Frequently Asked Questions (FAQs)
What is abnormal head posture and why does it happen?
Abnormal head posture refers to consistently tilting, turning, or angling the head while focusing on objects. This behavior usually develops as a natural adjustment to improve visual clarity or reduce discomfort. It may occur when the eyes are not aligned properly, when vision differs between the eyes, or when eye movement is unstable. In some cases, muscular or neurological factors contribute as well. Because the posture is often compensatory rather than intentional, identifying the underlying cause is important. Proper evaluation allows targeted abnormal head posture treatment to address the source of the issue rather than simply correcting the visible positioning.
What is ocular torticollis?
Ocular torticollis is a condition where a person adopts an unusual head position to optimize vision. Instead of being caused by neck problems, the posture stems from visual factors such as eye alignment differences or focusing issues. By adjusting the head position, the brain improves visual coordination or clarity. Although this adaptation may help short-term vision, it indicates that something within the visual system needs attention. Management focuses on diagnosing and treating the underlying cause so that the head can return to a natural position without sacrificing visual comfort or performance.
How can I tell if abnormal head posture requires evaluation?
Occasional posture adjustments are normal, but persistent or noticeable head tilting or turning should be assessed. Signs that evaluation may be helpful include recurring neck discomfort, double vision, headaches, eye strain, or difficulty focusing. In children, consistent head positioning during reading or screen use can signal an issue even if no complaints are expressed. Because abnormal head posture often compensates for visual challenges, ignoring it may allow underlying problems to worsen. A comprehensive assessment helps determine whether treatment is needed and prevents long-term complications associated with uncorrected visual or musculoskeletal factors.
Can abnormal head posture affect long-term health?
Yes, prolonged abnormal positioning can lead to physical and visual consequences over time. Continuous strain on neck muscles may result in discomfort, tension, or chronic pain. In growing children, persistent tilt may influence facial or skeletal development. From a visual standpoint, untreated underlying conditions may reduce efficiency or clarity in everyday tasks. Addressing the root cause early can prevent these complications. Treatment not only improves posture but also supports balanced development, comfort, and visual stability, making early intervention beneficial for both physical and functional well-being.
What conditions commonly cause ocular torticollis?
Ocular torticollis can arise from several visual factors. Misalignment between the eyes, unstable eye movements, unequal visual strength, eyelid obstruction, or uncorrected focusing issues may lead individuals to adjust their head position. These adaptations help reduce visual conflict or improve clarity. However, posture changes may also stem from non-visual causes such as muscular or structural differences. Because many potential contributors exist, identifying the exact cause requires professional evaluation. Accurate diagnosis ensures treatment focuses on the appropriate underlying factor rather than addressing symptoms alone.
What treatments are available for abnormal head posture?
Treatment depends entirely on the cause identified during assessment. Options may include corrective lenses, visual training techniques, temporary occlusion methods, or procedures designed to improve alignment or coordination between the eyes. When posture originates from muscular issues, rehabilitation exercises may be recommended. Some individuals benefit from combining approaches for optimal outcomes. The goal of treatment is to restore natural positioning while improving visual comfort and function. Personalized planning ensures interventions address specific needs and support long-term results rather than short-term symptom management.
Is abnormal head posture common in children?
Yes, abnormal head posture frequently appears in children because they adapt quickly to visual challenges. Young individuals may tilt or turn their heads without recognizing that their vision is affected. This makes observation important, especially during activities like reading or screen use. Early identification allows timely management and supports proper visual development. Addressing underlying causes helps prevent potential physical or developmental complications. Monitoring posture patterns and seeking evaluation when changes persist ensures children receive appropriate guidance and support as their visual systems mature.
Can abnormal head posture correct itself?
In some mild cases, posture adjustments may resolve once temporary visual or physical factors improve. However, persistent positioning usually reflects an underlying issue that does not disappear without intervention. Assuming it will self-correct may delay necessary care and increase the risk of complications. Identifying contributing factors allows appropriate management and prevents unnecessary strain. Monitoring symptoms and seeking evaluation when posture changes remain consistent ensures the best chance for resolution and long-term comfort.
How is ocular torticollis diagnosed?
Diagnosis typically involves a detailed review of medical and visual history combined with clinical observation of posture and eye coordination. Measurements of head positioning, vision testing, and alignment assessments help determine whether posture adjustments improve visual function. Additional evaluations may assess eye movement patterns or focusing ability. The goal is to identify whether the posture is visually driven or related to other factors. Thorough assessment ensures treatment targets the underlying cause accurately, providing a foundation for effective management and improved outcomes.
Why is early treatment important?
Early management helps prevent both visual and physical complications. Addressing the root cause reduces strain on muscles, supports natural alignment, and improves overall visual efficiency. For children, timely intervention aids developmental balance and prevents structural changes that could occur over time. For adults, treatment can enhance comfort and productivity in daily tasks. Proactive care ensures issues are corrected before they become chronic or more complex to manage. Seeking evaluation at the first signs of persistent posture change supports lasting visual health and overall well-being.