Quick Links
- What Is a Detached Retina?
- Why a Detached Retina Is Serious
- Common Signs & Symptoms of a Detached Retina
- What Causes a Detached Retina?
- Diagnosing Retinal Detachment
- Treatment Options for Detached Retina
- What to Expect After Detached Retina Surgery
- Risks of Detached Retina Surgery
- Great External Resources
- Frequently Asked Questions (FAQs)
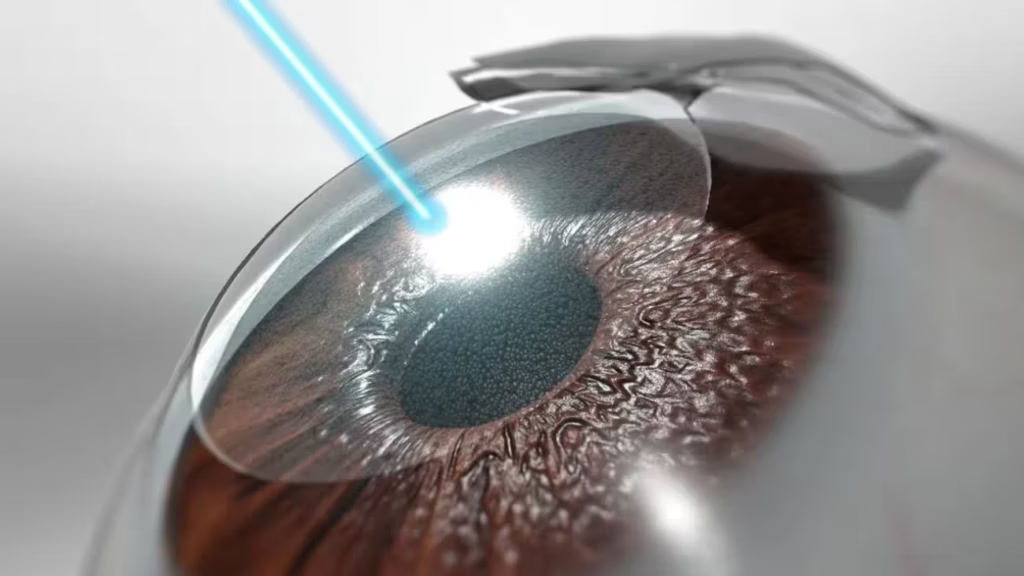
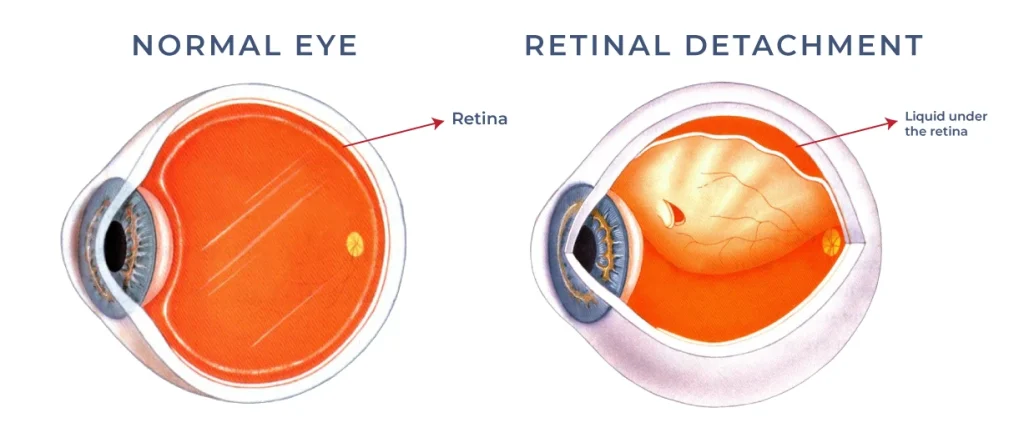
What Is a Detached Retina?
The retina is a delicate, essential tissue that lines the back of the eye. It converts light into electrical signals that the brain interprets as vision. When the retina detaches, its function is compromised because it no longer lies against its nourishing layers. This interruption can rapidly affect your sight.
A detached retina can occur suddenly or gradually. In either scenario, it is considered a medical emergency. Early intervention with expert detached retina diagnosis and surgery increases the chances of visual recovery and protects you from long‑term vision loss.
Why a Detached Retina Is Serious
When the retina lifts away from its underlying support, the eye loses its ability to send clear visual signals to the brain. Unlike minor eye irritations or temporary disturbances, a detached retina affects the fundamental structure of the eye. Without swift action:
Vision can deteriorate rapidly
Permanent scarring may occur
The retina may no longer reattach without surgery
If you notice warning signs of retinal detachment, immediate evaluation by an ophthalmologist is critical.
Common Signs & Symptoms of a Detached Retina
Detached retina symptoms often begin subtly and progress quickly. Recognizing these early warning signs can save your vision:
1. Sudden Flashes of Light
Seeing flashes — often described like stars after a camera flash — can indicate the retina is being tugged.
2. New or Increasing Floaters
You may notice specks, threads, or cobweb‑like shadows drifting through your vision.
3. Blurred Vision
As the retina begins to separate, your vision may become hazy or unclear.
4. Shadow or Curtain Over Vision
A common hallmark sign is a dark shadow spreading across your side (peripheral) vision, like a curtain falling over your field of sight.
5. No Pain
Unlike many eye issues, retinal detachment typically does not cause pain. Pain isn’t a reliable sign, so vision changes should never be ignored.
If you experience any of these symptoms — even if sight seems stable — seeking immediate evaluation is essential. Timely treatment can mean the difference between preserved vision and permanent loss.
What Causes a Detached Retina?
Understanding what causes a detached retina can help you identify risk factors and act quickly if warning signs appear.
1. Aging and Vitreous Changes
As we age, the vitreous (the clear gel that fills the eye) begins to shrink and liquefy. Sometimes it pulls on the retina with enough force to create a tear. Once a tear forms, fluid can slip behind the retina, causing a detachment.
2. Severe Nearsightedness (Myopia)
People with high degrees of nearsightedness are at greater risk because their eyeballs tend to be longer, and the retina is more stretched and susceptible to tears.
3. Eye Injury
Contact sports, accidents, or trauma to the eye can trigger retinal detachment.
4. Prior Eye Surgery
Previous procedures like cataract extraction may slightly increase the risk of detachment.
5. Family History
Genetics can play a role. If someone in your family has had a retinal detachment, your risk is higher.
6. Previous Retinal Tears
A history of retinal tears or lattice degeneration increases susceptibility.
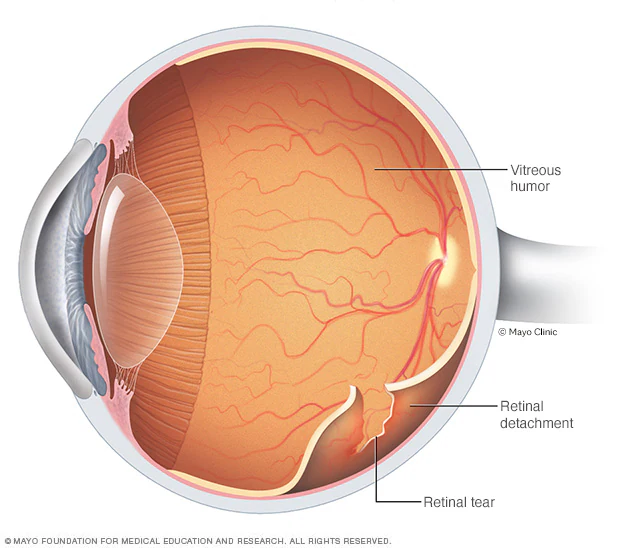
Diagnosing Retinal Detachment
Accurate and rapid diagnosis is essential to prevent permanent damage. Our specialists use a comprehensive eye examination to evaluate the retina:
Dilated Retinal Examination
Drops are placed in your eye to widen the pupil, allowing a detailed view of the retina with specialized lenses.
Ultrasound
If the view is obscured (e.g., by bleeding), ultrasound helps visualize the retina and guide treatment.
Prompt diagnosis ensures that treatment — often detached retina surgery — can be planned without delay.
Optical Imaging
High‑resolution imaging technologies like OCT (Optical Coherence Tomography) confirm the location and extent of the detachment.
Treatment Options for Detached Retina
Detached retina treatment depends on the severity, location, and pattern of the detachment. In many cases, detached retina surgery is necessary to reattach the retina and restore anatomical support.
Here are the most common and effective treatment methods:
1. Pneumatic Retinopexy
Pneumatic retinopexy is a minimally invasive office‑based procedure often used for small, uncomplicated detachments.
How It Works:
A small gas bubble is injected into the vitreous cavity.
The patient positions their head so the bubble floats against the detached retina, pushing it back into place.
Laser photocoagulation or cryotherapy (freezing) is applied to seal the retinal tear.
Benefits:
No major incision
Rapid recovery in select patients
However, strict post‑procedure positioning is critical for success.
2. Vitrectomy (Pars Plana Vitrectomy)
Vitrectomy is one of the most common surgeries for retinal detachment.
Procedure Overview:
The vitreous gel pulling on the retina is removed.
The space is filled with gas, air, or silicone oil to push the retina back into position.
Laser or freezing is used to secure the retina in place.
Silicone Oil vs. Gas:
Gas Bubble: Absorbs over time — no removal surgery needed.
Silicone Oil: May remain until a later time, requiring a second procedure.
Vitrectomy is effective for more complex or extensive detachments, including those involving scar tissue.
3. Scleral Buckling
Scleral buckle is a trusted method used for decades.
What Happens:
A flexible band (made of silicone or rubber) is sewn onto the sclera (white of the eye).
It gently indents the eye wall inward, bringing it closer to the detached retina.
This supports the retina externally and helps reattachment.
Scleral buckling can be used alone or in combination with vitrectomy.
What to Expect After Detached Retina Surgery
Recovery from detached retina surgery varies based on the procedure, but some general expectations include:
Post‑Surgery Vision
Vision may begin to improve within 4–6 weeks, though full stabilization can take several months. In some cases, vision continues to improve for up to a year as the retina heals.
Discomfort
Mild soreness or redness is common during the first few days. Your doctor can prescribe pain management as needed.
Head Positioning
If a gas bubble was used, strict head positioning will be required. This helps keep the bubble in the correct position to support healing.
Activity Restrictions
You may be advised to avoid:
Flying or high‑altitude travel
Scuba diving
Heavy lifting or intense physical exertion
These precautions prevent changes in pressure that could compromise healing.
Risks of Detached Retina Surgery
All surgeries carry potential risks. However, the risks of inaction — including permanent vision loss — are far greater. Common risks specific to detached retina surgery include:
1. Infection
In rare cases, the eye may develop an infection after surgery, usually treatable with antibiotics.
2. Bleeding
Minor bleeding during or after surgery is possible but typically resolves.
3. Increased Eye Pressure
Some patients may develop elevated intraocular pressure that needs monitoring and treatment.
4. Cataract Formation
Vitrectomy procedures can accelerate cataract development.
5. Need for Additional Surgery
Up to 1 in 20 patients may need a follow‑up procedure if the retina re‑detaches.
6. Re‑detachment
Despite surgery, there is a risk of recurrence, especially in complex cases.
Your surgeon will outline these risks and help you make an informed choice.
Great External Resources
Frequently Asked Questions (FAQs)
What does vision look like with a detached retina?
A detached retina can significantly affect your vision. People often describe seeing a sudden increase in floaters, flashes of light, or tiny specks that weren’t there before. Some notice a dark shadow or “curtain” moving across part of their visual field. Vision may also become blurry or distorted, and it can affect one eye at a time. The severity depends on how much of the retina is detached and how quickly treatment is received. Early detection is crucial because the longer the retina remains detached, the higher the risk of permanent vision loss.
What causes a detached retina?
A detached retina occurs when the retina, the thin light-sensitive layer at the back of the eye, separates from the underlying supportive tissue. This can happen due to aging changes in the vitreous gel inside the eye, eye injuries, or after eye surgery. People who are highly nearsighted, have had cataract or glaucoma surgery, or have a family history of retinal detachment are at higher risk. Sometimes, the vitreous pulls on a weak spot in the retina, causing a tear, and fluid can then accumulate behind it, leading to detachment. Prompt medical evaluation is essential to prevent permanent vision loss.
What does a detached retina feel like?
A detached retina usually does not cause pain. Unlike eye infections or injuries, the main signs are visual rather than physical discomfort. People may notice sudden flashes of light, new floaters, blurred vision, or a dark shadow across their vision. Some describe the sensation as a “curtain” over part of their sight. While it may feel alarming, the lack of pain can sometimes delay seeking treatment, which is risky. If you experience any sudden changes in vision, it is important to see an ophthalmologist immediately, as early intervention can save sight.
How is a detached retina diagnosed?
A detached retina is diagnosed through a comprehensive eye examination by an ophthalmologist. Eye drops are used to dilate (widen) the pupil, allowing the doctor to view the retina with a specialized lens. Imaging tests like optical coherence tomography (OCT) may also be used to assess the extent of detachment. The ophthalmologist will look for retinal tears, fluid accumulation, and other changes in the retina. Early diagnosis is critical because prompt surgical treatment greatly increases the chances of restoring vision and preventing permanent damage. If you notice flashes, floaters, or vision shadows, seek immediate evaluation.
How is a detached retina treated?
Treatment for a detached retina usually involves surgery, which is the only way to prevent permanent vision loss. Common procedures include pneumatic retinopexy, where a gas bubble is injected to push the retina back into place, vitrectomy, which removes vitreous gel pulling on the retina, and scleral buckle surgery, which uses a silicone band to support the retina. Laser therapy or cryotherapy may also seal retinal tears. Recovery depends on the type of surgery, the extent of detachment, and how quickly treatment is provided. Early surgical intervention offers the best chance of vision restoration.
How common is a detached retina?
Detached retina is relatively uncommon but becomes more likely with age or in people with certain risk factors. It is more frequent in individuals who are highly nearsighted, have had eye surgeries such as cataract removal, experienced severe eye trauma, or have a family history of retinal detachment. Studies estimate that approximately 1 in 10,000 people experience retinal detachment each year, but the risk increases with age, particularly in people over 50. Prompt awareness of warning signs, such as flashes and floaters, is essential for timely treatment and to prevent permanent vision loss.
Can a detached retina be fixed?
Yes, a detached retina can often be repaired successfully with surgery, but prompt treatment is essential. The type of surgery depends on the severity and location of the detachment. Procedures like vitrectomy, scleral buckle, or pneumatic retinopexy can reattach the retina and restore vision to varying degrees. While most patients regain some vision, the amount recovered depends on how quickly the retina was treated and whether the macula, the central part of the retina, was involved. Delaying treatment increases the risk of permanent vision loss, so early evaluation by an ophthalmologist is crucial.
Can a detached retina cause blindness?
Yes, if left untreated, a detached retina can lead to permanent blindness in the affected eye. The retina is essential for converting light into visual signals, and once it detaches from the underlying tissue, it cannot function properly. The risk of permanent vision loss is higher if the detachment affects the central retina (macula). Early detection and prompt surgical treatment are key to preserving vision. Even after successful surgery, some vision may remain impaired, depending on how long the retina was detached before treatment.
Can a detached retina heal on its own?
No, a detached retina cannot heal by itself. Once the retina separates from its underlying tissue, it requires surgical intervention to reattach it. Without treatment, the retina cannot function, leading to permanent vision loss. Some minor retinal tears may be managed with laser therapy if detected early, but complete detachment always requires surgical repair. If you experience sudden flashes, floaters, or vision shadows, immediate consultation with an ophthalmologist is crucial. Early intervention gives the best chance of restoring vision and preventing permanent damage.
Can a detached retina cause dizziness?
While dizziness is not a direct symptom of retinal detachment, visual disturbances caused by the detachment can sometimes lead to disorientation or imbalance. Sudden changes in vision, blurred areas, or a shadow across the visual field can make navigating spaces difficult, which may be perceived as dizziness. If you experience any visual changes accompanied by dizziness, it is important to seek medical attention immediately to rule out retinal detachment or other serious eye conditions. Prompt diagnosis and treatment are essential for preserving vision.
Can a detached retina cause double vision?
A detached retina generally does not cause true double vision (diplopia). However, if the detachment affects peripheral vision or causes visual distortion, some patients may perceive overlapping images or blurred vision, which can feel similar to double vision. Double vision can also occur if retinal detachment is combined with other eye conditions affecting eye alignment or the cornea. Any new visual disturbances should be assessed immediately by an ophthalmologist to ensure timely diagnosis and treatment. Early intervention is crucial to prevent permanent vision loss.
Can the symptoms of a detached retina come and go?
Yes, in some cases, early symptoms like flashes of light or floaters may seem intermittent. However, this does not mean the detachment is resolving on its own. Retinal tears or small detachments can progress over hours or days, and any delay in treatment increases the risk of permanent vision loss. Even if symptoms temporarily appear mild or fade, immediate evaluation by an ophthalmologist is critical. Prompt detection and surgical repair are essential to prevent the retina from fully detaching and causing irreversible blindness.