Quick Links
- What Is Blepharitis?
- Types of Blepharitis
- Common Symptoms of Blepharitis
- What Causes Blepharitis?
- Risk Factors for Blepharitis
- How Blepharitis Is Diagnosed
- Blepharitis Treatment Options
- Lifestyle Changes That Support Blepharitis Treatment
- Blepharitis and Dry Eye Disease
- Is Blepharitis Curable?
- When to Seek Medical Care
- Long-Term Management of Blepharitis
- Great External Resources
- Frequently Asked Questions (FAQs)
What Is Blepharitis?
Blepharitis refers to inflammation of the eyelid margins — the area where the eyelashes grow. It commonly affects both eyes and can be chronic, meaning symptoms tend to come and go over time.
The eyelids contain tiny oil-producing glands called meibomian glands. These glands release oils that form part of your tear film, preventing tears from evaporating too quickly. When these glands become blocked or inflamed, blepharitis can develop.
It is not contagious and typically does not cause permanent vision loss. However, without proper blepharitis treatment, it can lead to ongoing discomfort and secondary eye problems.
Types of Blepharitis
Understanding the type of blepharitis is essential in determining the most effective treatment approach.
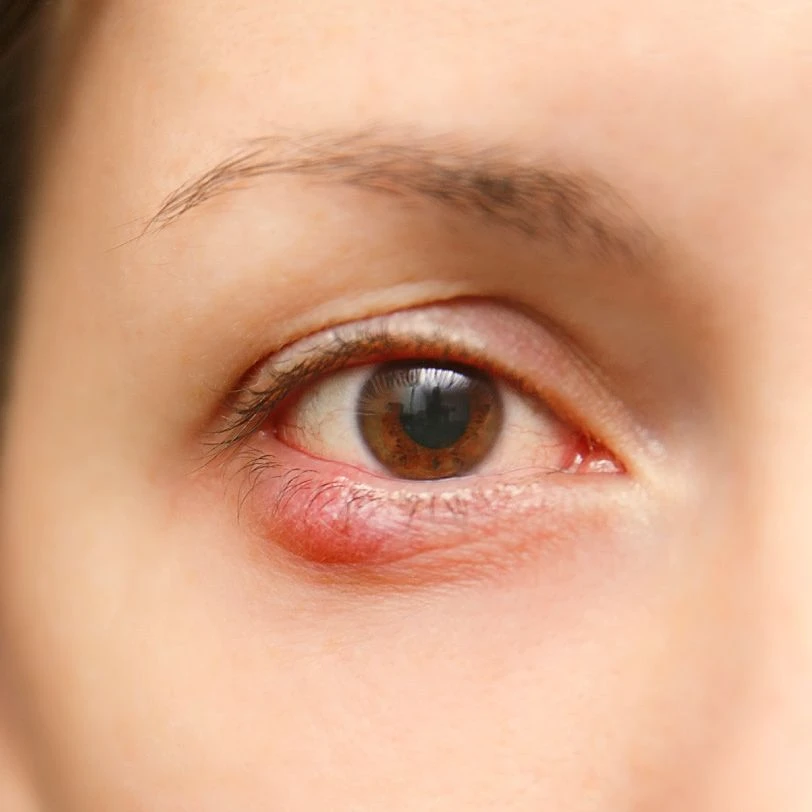
Anterior Blepharitis
Affects the outer front edge of the eyelid where eyelashes attach. It is often associated with:
Bacterial overgrowth (commonly Staphylococcus species)
Scalp dandruff (seborrheic dermatitis)
Skin debris buildup around lashes
Patients often notice flakes or crusting at the base of the eyelashes.
Posterior Blepharitis
Affects the inner eyelid margin and is linked to dysfunction of the meibomian glands. It is frequently associated with:
Meibomian gland dysfunction (MGD)
Rosacea
Oily skin conditions
Hormonal influences
Posterior blepharitis is one of the leading causes of evaporative dry eye disease.
Many patients experience a combination of both types, requiring a comprehensive blepharitis treatment strategy.
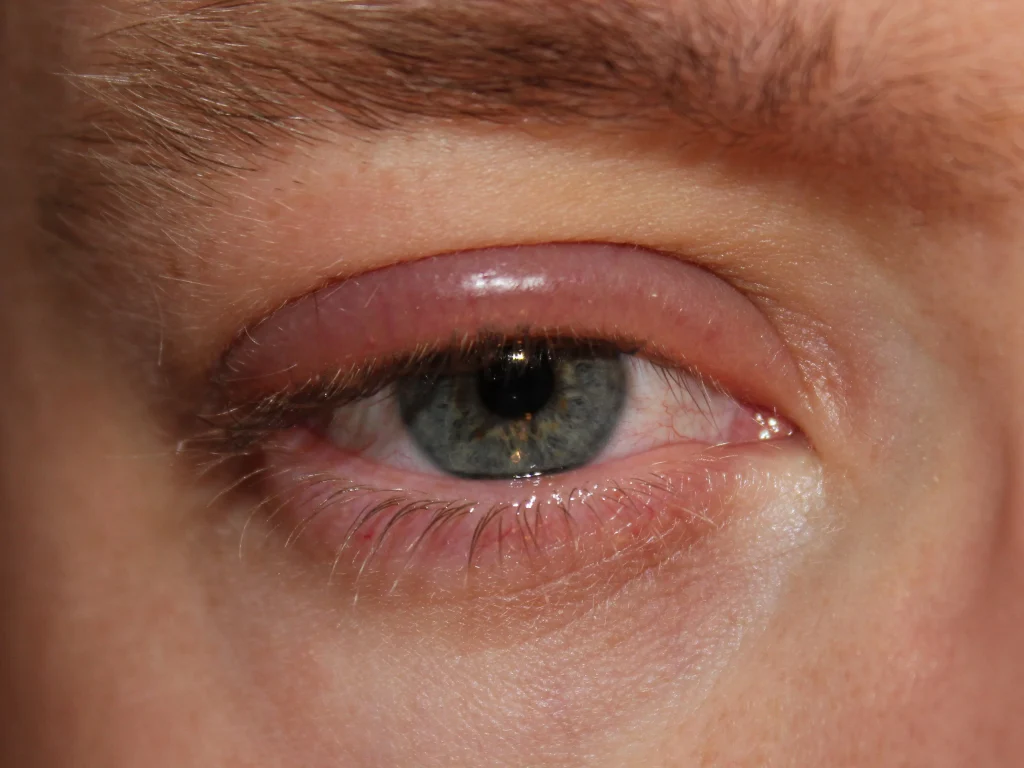
Common Symptoms of Blepharitis
Symptoms often fluctuate in severity. They may worsen during times of stress, illness, environmental changes, or poor eyelid hygiene.
Common symptoms include:
Red, swollen eyelids
Burning or stinging sensation
Itchy eyelids
Crusting or flakes at the base of lashes
Greasy eyelids
Eyelids sticking together upon waking
Foamy or bubbly tears
Watery eyes
Dry eye sensation
Light sensitivity
Blurred vision that improves with blinking
Symptoms are typically worse in the morning due to overnight debris buildup.
What Causes Blepharitis?
It develops when inflammation affects the eyelid margins. Several contributing factors may be involved:
Bacterial Overgrowth
Everyone naturally has bacteria on their skin. In some individuals, bacteria multiply excessively at the base of the eyelashes, triggering inflammation.
Meibomian Gland Dysfunction (MGD)
When oil glands become clogged or produce poor-quality oil, the tear film becomes unstable, contributing to irritation and inflammation.
Skin Conditions
Certain dermatologic conditions increase the risk of blepharitis:
Seborrheic dermatitis (dandruff)
Acne rosacea
Oily skin disorders
Demodex Mites
Microscopic mites known as Demodex can live in eyelash follicles. In high numbers, they may contribute to chronic blepharitis.
Allergic Reactions
Reactions to eye makeup, contact lens solutions, or eye medications may worsen inflammation.
Blepharitis is often multifactorial, meaning several causes may contribute at once.

Risk Factors for Blepharitis
Certain individuals are more prone to developing blepharitis:
People with rosacea
Individuals with dandruff or oily skin
Patients with dry eye syndrome
Contact lens wearers
Individuals with autoimmune conditions
Those with poor eyelid hygiene habits
Recognizing risk factors helps guide preventive treatment strategies.
How Blepharitis Is Diagnosed
Diagnosis is typically made through a comprehensive eye examination.
An evaluation may include:
Review of symptoms and medical history
Slit-lamp examination to assess eyelid margins
Evaluation of meibomian gland openings
Examination of tear film quality
Identification of debris, crusting, or lash abnormalities
In persistent or severe cases, additional testing may be performed to rule out other eyelid disorders.
Blepharitis Treatment Options
Although there is no permanent cure, consistent blepharitis treatment can successfully control symptoms and prevent flare-ups.
Treatment usually combines at-home care and medical therapies.
Warm Compress Therapy
Warm compresses are a cornerstone of treatment.
Applying a warm compress to closed eyelids for 5–10 minutes:
Softens hardened oils
Loosens crusts and debris
Improves meibomian gland function
Reduces gland blockage
Consistency is critical. Daily use is often recommended for chronic blepharitis.
Eyelid Cleansing and Hygiene
Eyelid hygiene is essential for long-term control.
Daily cleansing helps remove:
Bacteria
Oil buildup
Skin flakes
Debris around lashes
Cleansing options may include:
Diluted baby shampoo
Saline solution
Commercial eyelid wipes
Antiseptic lid cleansers
Gentle scrubbing along the lash line helps reduce inflammation and bacterial load.
Artificial Tears
Blepharitis often disrupts the tear film, leading to dryness and irritation.
Artificial tears can:
Improve moisture
Stabilize the tear film
Reduce burning and grittiness
Preservative-free formulations are typically preferred for frequent use.
Antibiotic Therapy
Antibiotics may be prescribed for certain forms of blepharitis.
Options include:
Topical antibiotic ointments
Oral antibiotics (such as doxycycline) for rosacea-related blepharitis
Oral antibiotics may also help improve meibomian gland function by reducing inflammation.
Anti-Inflammatory Medications
Short-term steroid eye drops may be used to reduce severe inflammation. However, long-term steroid use is avoided due to risks such as glaucoma or cataracts.
Other prescription anti-inflammatory drops may be recommended in chronic cases.
In-Office Thermal Treatments
Advanced blepharitis treatment options may include thermal pulsation or heat-and-massage devices performed in-office. These treatments:
Unclog meibomian glands
Improve oil flow
Reduce inflammation
Provide longer-lasting relief
These therapies are particularly helpful for posterior blepharitis associated with gland dysfunction.
Omega-3 Supplementation
Omega-3 fatty acids may help improve oil gland function and reduce inflammation.
Sources include:
Salmon
Sardines
Flaxseed
Fish oil supplements
Patients should consult their healthcare provider before starting supplements.
Lifestyle Changes That Support Blepharitis Treatment
Managing it requires ongoing lifestyle adjustments.
Avoid Eye Makeup During Flare-Ups
Cosmetics can worsen inflammation and block glands.
Replace Eye Makeup Regularly
Old mascara and eyeliner can harbor bacteria.
Avoid Contact Lenses During Active Symptoms
Contacts may worsen irritation.
Maintain Scalp and Skin Health
Treat dandruff or rosacea promptly.
Improve Environmental Factors
Use humidifiers and reduce exposure to smoke or irritants.
Blepharitis and Dry Eye Disease
It is one of the most common causes of evaporative dry eye.
When meibomian glands fail to produce adequate oil:
Tears evaporate too quickly
Eyes become dry and irritated
Vision may fluctuate
Treating blepharitis often improves dry eye symptoms dramatically.
Is Blepharitis Curable?
It is considered a chronic condition. There is no permanent cure, but symptoms can be effectively managed.
Most patients require ongoing eyelid hygiene to maintain control. When treatment is consistent, flare-ups become less frequent and less severe.
When to Seek Medical Care
Seek professional evaluation if you experience:
Persistent symptoms despite home care
Eye pain
Significant vision changes
Severe redness
Light sensitivity
Frequent styes or chalazia
Early treatment prevents complications and improves long-term comfort.
Long-Term Management of Blepharitis
The key to successful blepharitis treatment is consistency.
A typical long-term plan may include:
Daily warm compresses
Routine eyelid cleansing
Artificial tears
Periodic medical evaluation
Management of underlying skin conditions
With proper care, most individuals can live comfortably and maintain healthy vision.
Great External Resources
Frequently Asked Questions (FAQs)
Can blepharitis be cured?
It is a chronic condition, meaning there is no permanent cure. However, it can be effectively managed with proper eyelid care. Regular cleaning, warm compresses, and medications prescribed by an eye care professional can control symptoms and prevent flare-ups. Lifestyle factors such as reducing exposure to dust, managing underlying skin conditions, and using omega-3 supplements may further help maintain healthy eyelids.
Can blepharitis cause blindness?
While it rarely threatens vision, untreated or severe cases may cause complications that affect the eyes. Chronic inflammation can lead to corneal damage, persistent dry eye, or misdirected eyelashes, which can irritate the cornea. With early diagnosis and consistent treatment, the risk of vision problems is extremely low. Regular check-ups ensure that any complications are caught early.
Can blepharitis lead to styes?
Yes. Styes are small, painful lumps caused by bacterial infections in the oil glands of the eyelids. Since blepharitis involves bacterial overgrowth and inflammation of these glands, it creates an ideal environment for styes to develop. Maintaining eyelid hygiene with warm compresses and gentle scrubbing can significantly reduce the risk.
Can blepharitis be caused by allergies?
Allergies can worsen blepharitis by triggering inflammation and irritation in the eyelids. Allergic reactions to pollen, dust, makeup, or contact lens solutions can mimic or exacerbate blepharitis symptoms. Identifying allergens and limiting exposure, combined with eyelid hygiene, helps reduce flare-ups and discomfort.
Can blepharitis spread from one person to another?
It is not contagious. It is caused by bacteria naturally present on the eyelids or by gland dysfunction and skin conditions. While you cannot “catch” blepharitis from someone else, practicing good hygiene prevents worsening or recurring symptoms. Avoid sharing towels, pillows, or makeup during flare-ups as a general precaution.
Can blepharitis cause dry eye?
Yes, it is a common cause of dry eye syndrome. The inflammation interferes with the function of meibomian glands, which produce the oil layer of tears. Without this oil, tears evaporate too quickly, leaving the eyes dry, red, and irritated. Treatments like warm compresses, lid massages, artificial tears, and omega-3 fatty acids can improve tear quality and reduce dryness.
Can blepharitis cause eye pain?
It typically causes mild discomfort such as itching, burning, or a gritty sensation. Pain is usually mild but can increase if a secondary infection like a stye develops. Severe or persistent pain should prompt an eye care consultation to rule out other conditions. Regular eyelid care and avoiding rubbing the eyes help reduce discomfort.
Can blepharitis spread to the other eye?
Yes, it often affects both eyes because the underlying causes (bacterial overgrowth or gland dysfunction) are systemic. Even if only one eye shows symptoms initially, the other eye is at risk. Cleaning both eyelids regularly and following a consistent care routine reduces the likelihood of bilateral flare-ups.
Why does blepharitis come and go?
Symptoms fluctuate because the condition is chronic and influenced by external factors. Environmental triggers like dust, smoke, or seasonal allergies, as well as stress, diet, and inconsistent eyelid hygiene, can cause flare-ups. Understanding your triggers and maintaining a daily eyelid care routine helps minimize recurrence.
What should you avoid if you have blepharitis?
Managing it involves avoiding behaviors that worsen inflammation:
Avoid eye makeup during active flare-ups.
Do not rub or touch your eyes frequently.
Avoid contact lenses when eyelids are inflamed.
Stay away from harsh soaps, cleansers, or products that irritate the eyelid skin.
Limit exposure to dry, dusty, or smoky environments.
What can I do to avoid blepharitis
Daily eyelid hygiene: Warm compresses and gentle scrubs remove debris and unclog glands.
Omega-3 fatty acids: Supplements or fatty fish improve oil gland function.
Humidifiers: Adding moisture to the air reduces dryness during winter months.
Avoid triggers: Identify and minimize environmental or cosmetic irritants.
Regular check-ups: Long-term blepharitis management benefits from ophthalmologist guidance.
When do I go to see a doctor?
Persistent redness or irritation despite home care.
Development of styes, chalazia, or severe eye pain.
Blurred vision or corneal irritation.
Recurrent flare-ups indicating chronic eyelid inflammation.
Early intervention can prevent complications and ensure better symptom control.
Can blepharitis affect contact lens wearers?
Yes, itcan make wearing contact lenses uncomfortable. The inflammation and oil gland dysfunction can cause dryness, irritation, and a gritty sensation, which may worsen with contacts. If you wear lenses, it’s important to follow strict eyelid hygiene, use lubricating drops, and consider switching to daily disposable lenses during flare-ups. Always consult your eye care professional before resuming contact lens use if symptoms are active.
Can diet affect blpeharitis?
Yes, diet can influence eyelid and gland health. Omega-3 fatty acids, found in fish oil, flaxseed, and walnuts, support healthy oil gland function. Limiting processed foods, sugar, and inflammatory foods may also reduce eyelid inflammation. Hydration is important, as it helps maintain tear film quality and prevents excessive dryness.