Quick Links
- What Is Glaucoma?
- Who Is at Risk for Glaucoma?
- Types of Glaucoma and What They Mean for Your Vision
- Symptoms of Glaucoma
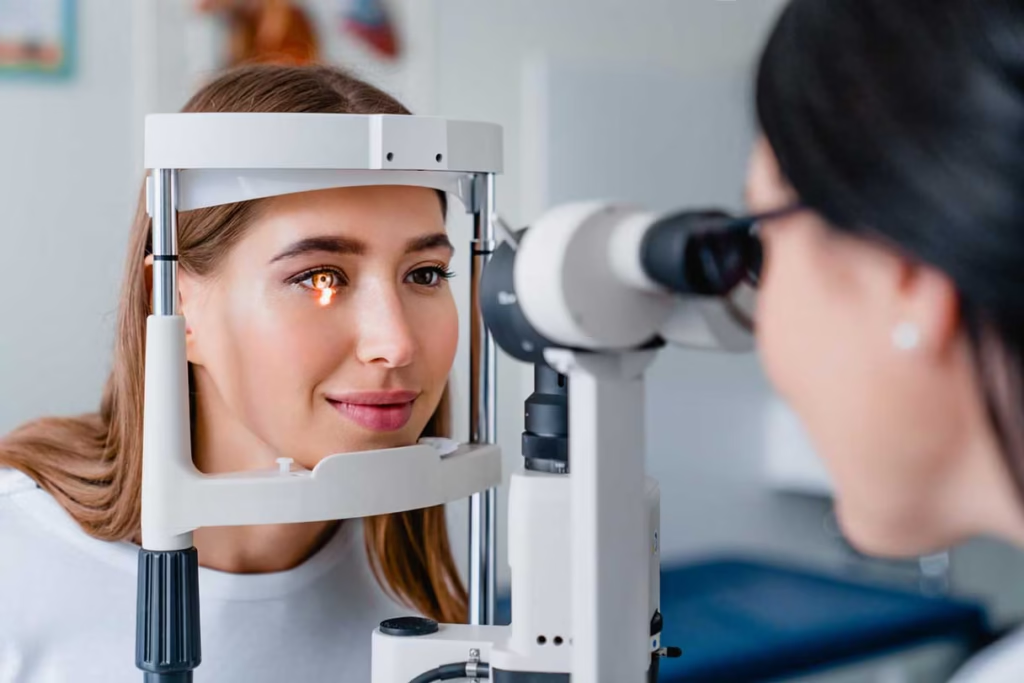
- How Glaucoma Is Diagnosed
- Glaucoma Treatment
- What to Expect During and After Glaucoma Surgery
- Managing Glaucoma for Life
- Great External Resources
- Frequently Asked Questions (FAQs)
What Is Glaucoma?
Glaucoma is an umbrella term for eye diseases that cause damage to the optic nerve — the bundle of more than one million nerve fibers that carry visual information to the brain. This damage is usually linked to elevated intraocular pressure (IOP), although some people develop glaucoma even within normal pressure ranges.
Under normal conditions, the eye makes fluid (aqueous humor) that flows through the front part of the eye and drains out through a structure called the drainage angle. If this drainage is blocked or inefficient, pressure builds up, compressing the optic nerve and leading to vision loss.
Because peripheral vision is affected first and symptoms may not appear until significant damage has occurred, glaucoma is often called the “silent thief of sight.” Early diagnosis and treatment are the best defenses against vision loss.
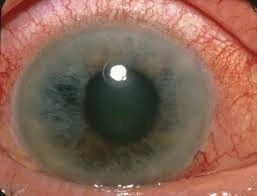
Who Is at Risk for Glaucoma?
Certain factors increase the likelihood of developing glaucoma. You are at higher risk if you:
Are over age 40
Have a family history of glaucoma
Have high eye pressure (ocular hypertension)
Have thin corneas
Are nearsighted or farsighted
Have diabetes, hypertension, or poor blood circulation
Are of African, Hispanic, or Asian heritage
Have had eye trauma or long‑term steroid use
Because many people with glaucoma have no early symptoms, regular eye exams are essential — especially if you have one or more risk factors. Early detection allows for early glaucoma treatment that preserves vision.
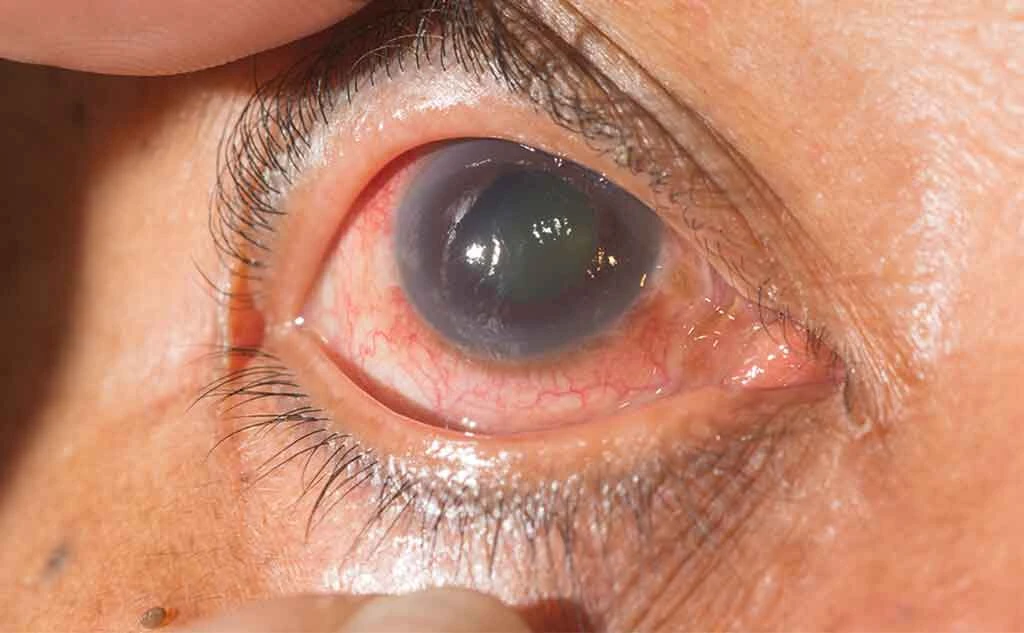
Types of Glaucoma and What They Mean for Your Vision
Open‑Angle Glaucoma
This is the most common form of glaucoma. The drainage angle remains open, but fluid leaves the eye too slowly, causing pressure to build gradually. There are usually no early symptoms, and vision loss begins peripherally, which patients may not notice until the disease is advanced.
Angle‑Closure Glaucoma
Also called narrow‑angle glaucoma, this type occurs when the iris blocks fluid drainage entirely, causing pressure to rise quickly. It can present suddenly with severe eye pain, blurred vision, headaches, nausea, and seeing halos around lights. This is a true eye emergency requiring immediate treatment to prevent permanent vision loss.
Normal‑Tension Glaucoma
In this form, optic nerve damage occurs even when eye pressure is within a normal range. Normal‑tension glaucoma typically requires careful monitoring and often more aggressive treatment to protect vision.
Secondary and Congenital Glaucoma
Other eye conditions, medications (like corticosteroids), or injuries can lead to secondary glaucoma. Congenital glaucoma occurs in infants and requires early intervention.
Symptoms of Glaucoma
In the early stages, many forms of glaucoma cause no noticeable symptoms. Over time, glaucoma can produce:
Gradual loss of peripheral (side) vision
Blurred or hazy vision
Blind spots
Difficulty seeing in low light
Halos around lights
Red or bloodshot eyes
Headaches or eye discomfort (especially with angle‑closure glaucoma)
Sudden vision changes requiring immediate care
When pressure rises quickly — as in acute angle‑closure glaucoma — symptoms can include severe pain, nausea, vomiting, and rainbow‑colored circles around lights. These require urgent medical attention to prevent irreversible damage.
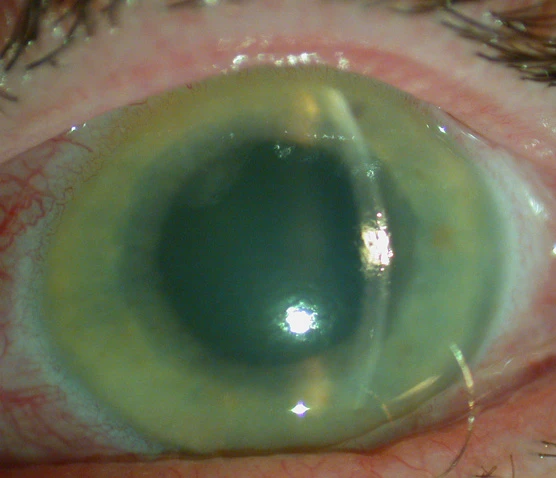
How Glaucoma Is Diagnosed
A comprehensive eye examination is essential for diagnosing glaucoma. A single pressure test alone is not sufficient; glaucoma diagnosis involves multiple components:
Tonometry – Measures intraocular pressure
Optic Nerve Evaluation – Examines damage to the optic nerve
Visual Field Testing – Detects blind spots and peripheral vision loss
Gonioscopy – Evaluates the drainage angle
Corneal Thickness Measurement (Pachymetry) – Determines corneal properties
Optical Coherence Tomography (OCT) – High‑resolution imaging of retinal and nerve layers
Regular eye exams with a glaucoma specialist can catch early signs of damage before you notice vision changes, increasing the chance of successful long‑term management.
Glaucoma Treatment
While glaucoma damage is permanent and cannot be reversed, glaucoma treatment can prevent further progression and preserve vision. Treatment is tailored to your type of glaucoma, disease stage, age, overall health, and lifestyle.
Medicated Eye Drops
Eye drops are often the first line of treatment. They lower intraocular pressure by reducing fluid production or improving fluid outflow. Common classes include:
Prostaglandin analogs
Beta blockers
Alpha agonists
Carbonic anhydrase inhibitors
Combination medications
Eye drops require consistent daily use. Patients must follow instructions carefully and report any side effects to their ophthalmologist.
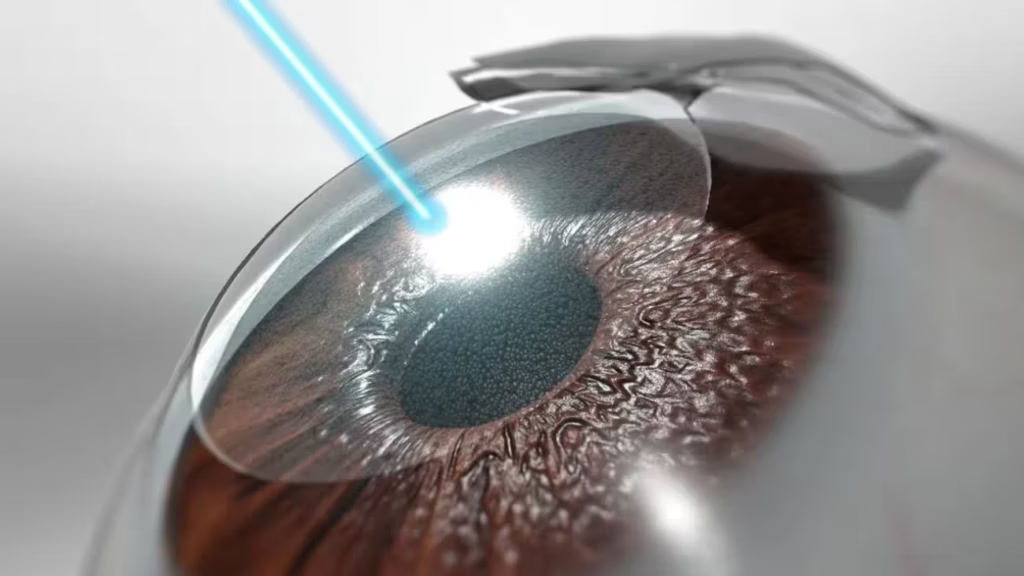
Laser Therapy
Laser treatments help improve aqueous humor drainage and lower intraocular pressure:
Laser Trabeculoplasty – Enhances fluid outflow in open‑angle glaucoma.
Laser Iridotomy – Creates a small opening in the iris to relieve fluid blockage in angle‑closure glaucoma.
These outpatient procedures are quick and often performed without the need for general anesthesia.
Minimally Invasive Glaucoma Surgery (MIGS)
MIGS procedures are newer surgical options that lower eye pressure with fewer risks and faster recovery compared to traditional surgery. MIGS is often used alongside cataract surgery in patients who have both conditions.
Traditional Glaucoma Surgery
When medications and laser treatments can’t sufficiently control eye pressure, surgery may be the best option:
Trabeculectomy – Creates a new drainage channel to allow fluid exit and lower pressure.
Glaucoma Drainage Devices (Tube Shunts) – Implants that establish a controlled pathway for fluid drainage.
Cataract Surgery – Sometimes recommended for narrow‑angle glaucoma to improve drainage by removing the natural lens.
Your ophthalmologist will discuss the most suitable surgical option based on your specific situation.
What to Expect During and After Glaucoma Surgery
Most glaucoma surgeries effectively lower intraocular pressure and slow disease progression. Recovery varies by procedure:
A short period of mild discomfort or redness
Temporary vision changes
Instructions for medicated eye drops and activity modifications
Post‑operative follow‑ups to monitor pressure and healing
Your doctor will guide you on when you can resume daily activities, drive, or exercise. Early reporting of symptoms such as increased pain or vision changes helps ensure the best outcome.
Managing Glaucoma for Life
Glaucoma is a chronic condition — lifelong monitoring and treatment are often necessary. Successful management is a partnership between you and your eye care team. Key components include:
Consistent use of prescribed medications
Regular follow‑up visits every 3–6 months (or as advised)
Monitoring for side effects and vision changes
Maintaining overall health (healthy diet, exercise, blood pressure control)
Awareness of risk factors and early symptoms
Following your treatment plan significantly lowers the risk of severe vision loss and allows most people with glaucoma to live full, active lives.
Great External Resources
Frequently Asked Questions (FAQs)
What does glaucoma look like?
The condition itself does not have any external appearance that others can notice. Unlike eye problems that cause redness, swelling, or irritation, most forms progress silently within the eye. The optic nerve — which carries visual information from the eye to the brain — gradually degenerates, often without any outward signs. Peripheral vision may slowly narrow over time, something patients usually do not recognize in the early stages. In advanced cases, tunnel vision may develop, where only central vision remains intact, giving the impression of looking through a narrow tube.
The only way to detect changes is through comprehensive eye examinations. Eye care specialists use specialized imaging, tonometry, and visual field tests to assess optic nerve health and monitor disease progression. Early detection is essential because vision loss is permanent. Treatment focuses on controlling eye pressure and preventing further damage rather than restoring lost sight, making regular checkups and timely intervention critical to preserving long-term vision.
What does glaucoma feel like?
In most cases, the condition is painless, which is why it is often called the “silent thief of sight.” Patients with open-angle types typically feel no discomfort as the disease progresses, making it difficult to recognize without regular eye exams. In contrast, angle-closure forms can produce sudden and intense eye pain, headaches, nausea, and even vomiting, requiring immediate medical attention to prevent permanent vision loss.
Some individuals may notice subtle visual disturbances, such as halos around lights or mild blurred vision, especially in low-light conditions. These sensations can indicate rising eye pressure or optic nerve stress. Because most cases are symptom-free until significant damage occurs, regular screening is essential, particularly for people with risk factors such as a family history, elevated eye pressure, or age over 40. Early detection and consistent monitoring are key to preserving vision and preventing severe complications.
What should glaucoma patients avoid?
Patients should avoid activities and habits that can increase eye pressure. This includes holding the breath while straining, lifting very heavy weights incorrectly, or engaging in exercises that dramatically raise intraocular pressure. Certain medications, particularly steroids, may also raise eye pressure if used without supervision. Lifestyle factors such as smoking, excessive alcohol consumption, and poorly controlled conditions like hypertension or diabetes can further compromise eye health and accelerate progression.
It is also essential not to skip prescribed medications or eye drop routines. Missing doses can lead to uncontrolled pressure, increasing the risk of optic nerve damage. Wearing protective eyewear helps prevent injuries that could worsen the condition or lead to secondary complications. Regular checkups and careful monitoring of eye pressure and overall health are key to minimizing risks and preserving vision.
What makes glaucoma worse?
The condition worsens primarily when intraocular pressure remains elevated and uncontrolled. Factors like irregular medication adherence, missed appointments, or untreated risk factors such as high blood pressure or diabetes can accelerate optic nerve damage. Eye injuries, chronic inflammation, and certain medications — especially corticosteroids — may also exacerbate the problem.
Lifestyle choices can contribute as well. Heavy straining, improper lifting, or activities that temporarily increase eye pressure may add stress to the optic nerve over time. Lack of awareness or delayed diagnosis allows the disease to progress silently, making regular eye exams and early intervention essential to prevent further vision loss. Consistent management of eye pressure and overall health is critical for slowing progression and maintaining quality of vision.
What happens when glaucoma drops don’t work?
Sometimes, eye drops alone are insufficient to control intraocular pressure. This can happen if the condition is advanced, if the optic nerve is highly sensitive to normal pressure, or if the medication fails to adequately lower eye pressure. Non-adherence or improper use of eye drops can also reduce their effectiveness.
When drops don’t work, ophthalmologists may recommend alternative treatments such as laser therapy, minimally invasive surgery (MIGS), or traditional surgical procedures like trabeculectomy. These interventions create new drainage pathways for fluid or improve existing ones, reducing pressure and preventing further optic nerve damage. Patients should not stop medications abruptly and must follow their doctor’s guidance closely.
When should glaucoma patients see a doctor?
Patients should see an ophthalmologist regularly, typically every 3–6 months, or as recommended by their eye care professional. Immediate medical attention is required if sudden vision changes, eye pain, blurred vision, halos, or nausea occur, which can signal an acute angle-closure attack.
Even in the absence of symptoms, routine follow-ups are critical. The condition can progress silently, and early detection of optic nerve changes or pressure fluctuations allows timely adjustments in treatment. Prompt medical care minimizes the risk of irreversible vision loss.
Why can’t glaucoma be cured?
The condition cannot be cured because it causes permanent damage to the optic nerve, which cannot regenerate. Unlike infections or temporary conditions, the nerve fibers responsible for transmitting visual signals to the brain, once damaged or lost, cannot be restored.
Treatment focuses on slowing or stopping progression rather than reversing the damage. Medications, laser procedures, and surgery aim to control intraocular pressure and protect remaining vision. Early detection and consistent management remain the most effective strategies to maintain quality of life and prevent blindness.
Can glaucoma be treated?
Yes, the condition can be treated. Treatment does not reverse existing damage but helps control intraocular pressure to prevent further optic nerve loss. First-line therapy typically involves prescription eye drops. If these are insufficient, laser procedures or surgery can improve fluid drainage and reduce pressure.
Successful treatment requires ongoing monitoring, medication adherence, lifestyle adjustments, and periodic visits with an ophthalmologist. With early diagnosis and consistent care, most patients can maintain functional vision and avoid severe vision loss.
Can glaucoma be cured by laser treatment?
Laser treatment cannot cure the condition, but it can be an effective way to lower intraocular pressure and prevent further optic nerve damage. Procedures like laser trabeculoplasty (for open-angle) or laser iridotomy (for angle-closure) improve fluid drainage and help stabilize eye pressure.
Laser therapy is often used when medications alone are insufficient or in combination with other treatments. While it does not restore lost vision, it is a minimally invasive option that can reduce reliance on eye drops and delay or prevent the need for more invasive surgery.