Quick Links
Understanding Diabetic Retinopathy
Diabetic retinopathy progresses in stages and may initially present without noticeable symptoms. Understanding these stages helps patients and caregivers recognize the importance of early treatment and regular eye exams:
1. Background (Non-Proliferative) Diabetic Retinopathy
At this stage, small blood vessels in the retina are damaged, but vision remains largely unaffected. Patients may have tiny hemorrhages or microaneurysms, but these often go unnoticed without a professional eye exam.
2. Pre-Proliferative Diabetic Retinopathy
As the disease progresses, more severe changes occur in retinal blood vessels. This stage carries a higher risk of vision loss in the future. While treatment may not yet be required, closer monitoring and frequent screenings are recommended to detect any changes early.
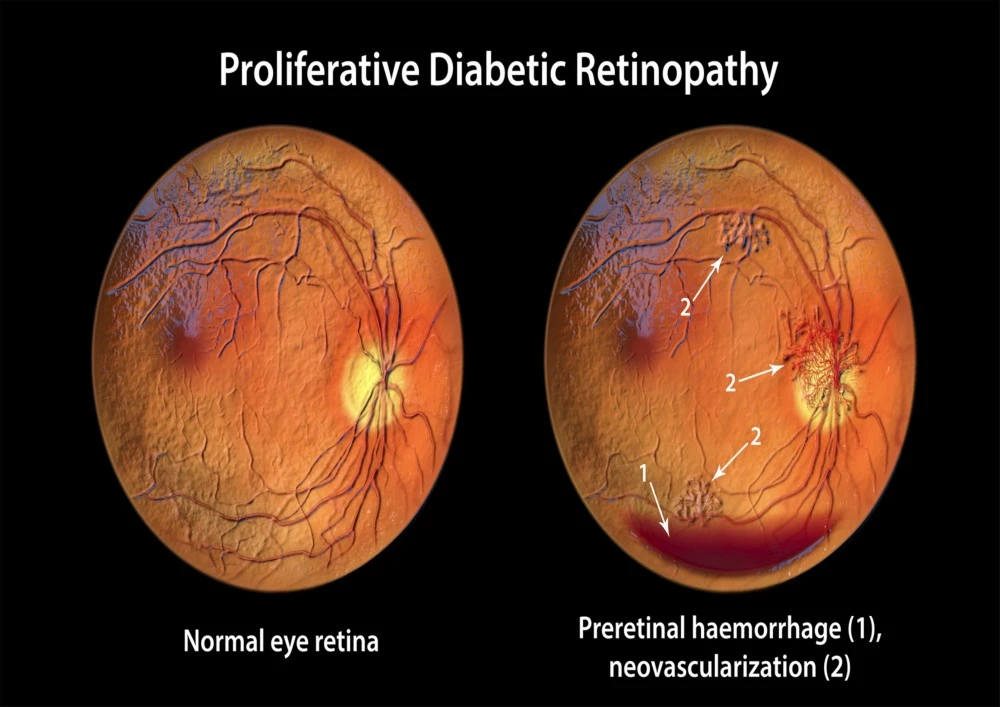
3. Proliferative Diabetic Retinopathy
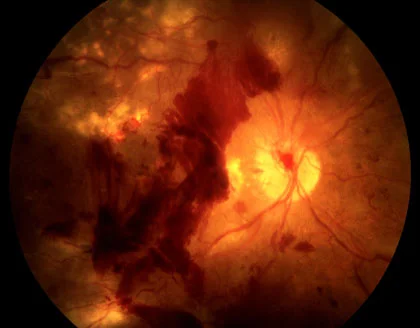
This advanced stage is characterized by the growth of abnormal new blood vessels (neovascularization). These vessels are fragile and prone to bleeding, which can lead to vitreous hemorrhages, retinal detachment, and severe vision impairment. Immediate consultation with a retina specialist is crucial at this stage.
4. Diabetic Maculopathy
When diabetic retinopathy affects the central retina, or macula, it is referred to as diabetic maculopathy or macular edema. This can cause blurred or distorted central vision, making reading, driving, and recognizing faces more difficult.
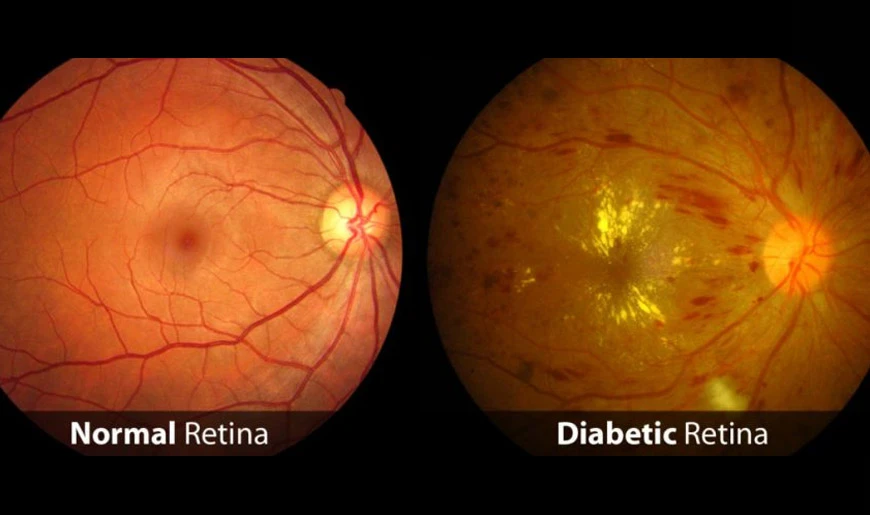
Symptoms of Diabetic Retinopathy
In early stages, diabetic retinopathy usually does not produce noticeable symptoms. As the disease progresses, patients may experience:
Blurred or fluctuating vision
Floaters (small spots or lines in vision)
Difficulty seeing at night or in low light
Vision loss in one or both eyes
If you experience sudden changes in vision, blurred sight, or a noticeable decrease in visual clarity, it is critical to seek immediate medical attention. Early intervention is the most effective way to prevent permanent vision loss.
Diagnosis of Diabetic Retinopathy
Early detection of diabetic retinopathy is vital for effective treatment. Comprehensive diagnostic testing includes:
1. Dilated Eye Exam
Eye drops are used to widen the pupils, allowing the specialist to examine the retina and optic nerve for signs of damage. This is the standard first step in diagnosis and monitoring.
2. Optical Coherence Tomography (OCT)
OCT produces detailed cross-sectional images of the retina, revealing any fluid buildup, swelling, or structural changes. This test helps guide treatment decisions and monitor therapy effectiveness over time.
3. Fluorescein Angiography
A dye is injected into a vein, and special photographs track its circulation through retinal blood vessels. This test identifies blocked, leaking, or abnormal vessels, guiding laser treatment or surgical intervention.
4. Routine Eye Screening
For people with diabetes, regular screenings are essential. Those with type 1 diabetes should have an initial exam within five years of diagnosis, while type 2 diabetes patients should be screened at the time of diagnosis. Screening intervals may vary based on disease severity and overall eye health.
Treatment Options
While diabetic retinopathy cannot be cured, effective treatments can prevent or delay vision loss. The choice of therapy depends on disease stage, symptoms, and overall health.
1. Medical Management
Controlling blood sugar, blood pressure, and cholesterol is the first line of defense. Patients benefit from consistent monitoring and lifestyle modifications, including diet, exercise, and smoking cessation. Tight glycemic control helps slow progression and supports the effectiveness of other treatments.
2. Anti-VEGF Injections
Medications such as aflibercept (Eylea) and ranibizumab (Lucentis) target vascular endothelial growth factor (VEGF), a protein responsible for abnormal blood vessel growth. These injections reduce swelling and prevent further neovascularization. Steroid implants may also be used to control inflammation and fluid buildup in the macula.
3. Laser Therapy (Photocoagulation)
Laser treatment seals leaking blood vessels and reduces abnormal vessel growth. Focal laser therapy treats macular edema, while scatter or pan-retinal laser therapy prevents proliferation in advanced cases. This procedure can help preserve peripheral vision and prevent further retinal damage.
4. Vitrectomy Surgery
Vitrectomy involves removing blood, scar tissue, or vitreous gel from the eye. It is indicated in cases of vitreous hemorrhage, retinal detachment, or severe scar formation. Surgery improves vision when damage is treatable and is performed under local or general anesthesia in a surgical setting.
Preventing Diabetic Retinopathy Progression
Prevention is critical, and patients can take an active role in protecting their vision:
Maintain optimal blood sugar levels with regular monitoring
Keep blood pressure and cholesterol within target ranges
Attend all scheduled diabetic eye screenings and follow-up appointments
Avoid smoking and maintain a healthy lifestyle
Communicate any changes in vision to your healthcare team promptly
Even after successful treatment, ongoing management is necessary. Diabetic retinopathy can progress silently, making continuous monitoring essential.
Living with Diabetic Retinopathy
Vision loss from diabetic retinopathy can be challenging both practically and emotionally. Support resources can help:
Low vision aids: Magnifiers, screen readers, and specialized devices enhance independence.
Support groups: Connecting with others facing similar challenges provides emotional and practical guidance.
Professional counseling: Therapists can help cope with anxiety or depression associated with vision changes.
Combining medical treatment with supportive care improves quality of life and helps patients adapt to vision changes.
When to Seek Medical Attention
Immediate medical evaluation is required if you notice:
Sudden blurred vision or floaters
Partial or total loss of vision
Eye pain, redness, or other unusual symptoms
Prompt action can prevent permanent damage and improve treatment outcomes. Routine eye exams, even in the absence of symptoms, remain the best defense against progression.
Risk Factors
Several factors increase the likelihood of developing diabetic retinopathy, including:
Duration of diabetes: The longer a person has diabetes, the higher the risk.
Poor blood sugar control: Fluctuating or elevated blood glucose accelerates damage to retinal blood vessels.
High blood pressure or cholesterol: These conditions can worsen vascular damage in the retina.
Pregnancy: Hormonal changes can increase the risk or severity of retinopathy.
Lifestyle factors: Smoking, sedentary behavior, and poor diet can contribute to progression.
Managing these risk factors alongside regular eye exams significantly reduces the chances of severe vision impairment.
Great External Resources
Frequently Asked Questions (FAQs)
What are the causes of diabetic retinopathy?
Diabetic retinopathy is caused by damage to the small blood vessels in the retina, primarily due to prolonged high blood sugar levels. Over time, elevated glucose can weaken vessel walls, cause leaks, or block blood flow, depriving the retina of oxygen and nutrients. Risk factors include the duration of diabetes, poorly controlled blood sugar, high blood pressure, high cholesterol, smoking, and pregnancy. People with type 1 or type 2 diabetes are susceptible, and the likelihood increases with age. Proper management of blood sugar, blood pressure, and cholesterol can significantly reduce the risk of developing this eye condition.
What are the symptoms of diabetic retinopathy?
Diabetic retinopathy often develops without noticeable symptoms in its early stages, which is why regular eye exams are critical. As the condition progresses, people may experience blurred vision, floaters (spots or lines in the vision), difficulty seeing at night or in dim light, and a gradual loss of central or peripheral vision. Some may notice colors appearing faded or distorted. Sudden vision changes, flashes of light, or partial vision loss indicate advanced retinopathy and require urgent attention. Early detection is key to slowing progression and protecting vision before permanent damage occurs.
How does diabetic retinopathy feel?
Most people with diabetic retinopathy do not feel pain in the early stages, which is why it is often called a “silent” eye disease. Some individuals may notice subtle visual changes, such as blurry vision, shadows, floaters, or difficulty seeing in low light. In advanced stages, particularly with proliferative retinopathy or macular edema, vision may become noticeably distorted, making everyday tasks like reading, driving, or recognizing faces challenging. Because there is little to no discomfort in the early phases, patients often remain unaware of the condition, making routine eye screenings essential for detection and timely treatment.
What treatments are available for diabetic retinopathy?
Treatment for diabetic retinopathy depends on the severity and type of the condition. Early-stage retinopathy may only require careful monitoring and strict blood sugar control. For more advanced cases, treatments include anti-VEGF injections to reduce fluid buildup and slow abnormal blood vessel growth, laser therapy (photocoagulation) to seal leaking vessels or prevent new vessel formation, and vitrectomy surgery to remove blood or scar tissue from the eye. While treatment cannot reverse existing vision loss, it can prevent further deterioration, preserve remaining vision, and significantly reduce the risk of severe complications like retinal detachment or blindness.
Can diabetic retinopathy be reversed?
Unfortunately, vision lost due to diabetic retinopathy cannot be fully reversed because damaged retinal tissue and blood vessels cannot regenerate. Treatment is focused on preventing further progression and preserving the vision that remains. Early intervention, through careful blood sugar management, laser therapy, injections, or surgery, can stabilize the condition and reduce the risk of additional damage. While some temporary improvements in vision may occur after reducing fluid buildup or treating macular edema, the underlying structural damage remains permanent. Prompt diagnosis and ongoing monitoring remain the most effective strategies to slow progression and protect long-term vision.
Can diabetic retinopathy cause blindness?
Yes, diabetic retinopathy can lead to blindness if left untreated. Advanced stages of the condition, such as proliferative retinopathy, involve the growth of fragile, abnormal blood vessels that may bleed into the eye or cause retinal detachment. Macular edema, where fluid builds up in the central retina, can also severely affect vision. Although vision loss cannot be reversed, timely interventions like laser therapy, injections, and surgery can significantly reduce the risk of blindness. Early detection through routine screenings and strict diabetes management is the most effective way to protect sight and prevent irreversible vision loss.
Can diabetic retinopathy improve?
Diabetic retinopathy itself does not fully resolve, as retinal damage is permanent. However, treatment can improve or stabilize certain symptoms. For example, anti-VEGF injections and laser therapy can reduce fluid accumulation, shrink abnormal vessels, and improve visual clarity in some cases. Maintaining tight blood sugar control, managing blood pressure, and adopting a healthy lifestyle can also slow progression and prevent further deterioration. While lost vision cannot be restored, these interventions can preserve existing vision, improve quality of life, and prevent complications such as blindness, making ongoing care and follow-up essential.
Can diabetic retinopathy cause headaches?
Diabetic retinopathy does not typically cause headaches directly. However, vision problems associated with the condition, such as blurred or fluctuating vision, eye strain, or difficulty focusing, may contribute to eye fatigue and tension headaches in some individuals. Rarely, increased eye pressure from complications like neovascular glaucoma may cause pain or headache. Most headaches are unrelated to diabetic retinopathy, but any sudden changes in vision accompanied by pain or headache should prompt urgent evaluation by an eye specialist to rule out advanced complications or other eye conditions.
Can diabetic retinopathy lead to retinal detachment?
Yes, diabetic retinopathy can increase the risk of retinal detachment, particularly in proliferative stages. Abnormal blood vessels may grow on the retina and form scar tissue. Over time, this tissue can contract, pulling the retina away from its normal position, causing traction retinal detachment. Symptoms may include sudden flashes of light, floaters, or a curtain-like shadow across vision. Retinal detachment is a serious complication that requires urgent surgical intervention, such as vitrectomy, to prevent permanent vision loss. Regular eye exams can detect early signs and allow timely treatment to reduce the risk of detachment.
Can diabetic retinopathy cause glaucoma?
Diabetic retinopathy can indirectly contribute to glaucoma, particularly neovascular glaucoma. In advanced stages, abnormal blood vessels may grow in the iris and drainage channels of the eye, increasing intraocular pressure. Elevated pressure can damage the optic nerve, leading to glaucoma. This form of secondary glaucoma is serious and requires prompt intervention, often combining medications, laser therapy, or surgery to control eye pressure. Managing diabetic retinopathy early and monitoring eye health can reduce the risk of developing glaucoma and other vision-threatening complications.
Can diabetic retinopathy be prevented?
While diabetic retinopathy cannot always be entirely prevented, its onset and progression can be significantly reduced through proactive management. Key preventive measures include maintaining tight blood sugar control, managing blood pressure and cholesterol, quitting smoking, exercising regularly, and attending all scheduled eye exams. Early diagnosis through diabetic eye screenings allows timely interventions that protect vision. Healthy lifestyle choices combined with consistent diabetes management are the most effective strategies to reduce the risk of developing retinopathy or slowing its progression, ultimately preserving long-term eye health.