Quick Links
- What Are Eye Allergies?
- Common Eye Allergy Symptoms
- Causes and Risk Factors of Eye Allergies
- Types of Eye Allergies
- Diagnosing Eye Allergies
- Managing and Preventing Eye Allergies
- Eye Allergy Treatment Options
- Understanding Eye Allergy Triggers in Detail
- Lifestyle and Home Strategies for Prevention
- Eye Allergies in Special Situations
- Potential Complications if Untreated
- Eye Allergy Treatment for Children
- Long-Term Prevention Strategies
- When to See an Allergist or Eye Specialist
- Great External Resources
- Frequently Asked Questions (FAQs)
What Are Eye Allergies?
Eye allergies, also called allergic conjunctivitis, occur when the immune system overreacts to normally harmless substances called allergens. Common triggers include pollen, dust mites, pet dander, mold, smoke, perfumes, cosmetics, certain medications, and even preservatives in eye drops. Some people may also react to foods, insect bites, or environmental irritants like diesel exhaust.
When allergens come in contact with your eyes, mast cells release histamine and other chemicals, causing redness, itching, swelling, and tearing. Unlike infectious conjunctivitis, eye allergies are not contagious. Symptoms can affect one or both eyes and often occur alongside nasal allergies like sneezing, congestion, or runny nose.
Common Eye Allergy Symptoms
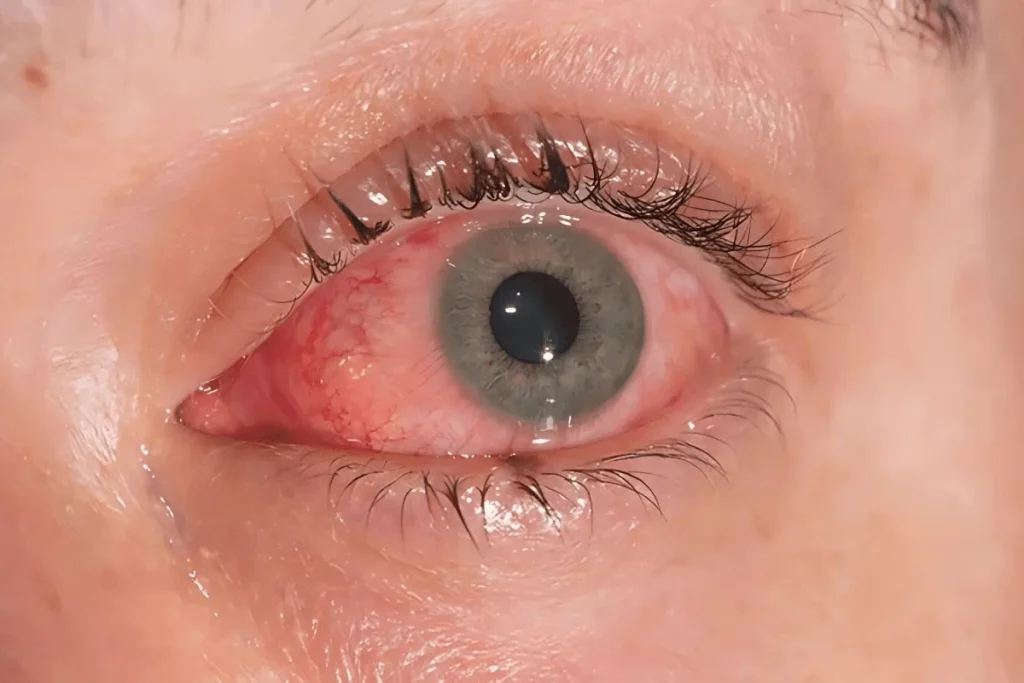
Recognizing symptoms early can prevent complications and guide proper treatment. Eye allergy symptoms range from mild irritation to severe discomfort:
Red, swollen, or itchy eyes
Burning or stinging sensations
Clear or watery discharge
Puffy or droopy eyelids
Feeling of a foreign object in the eye
Sensitivity to light (photophobia)
Blurred vision in severe cases
Chronic dark circles (“allergic shiners”)
Thick mucus discharge that may cause eyelids to stick
Some individuals may experience headaches, fatigue, or trouble sleeping due to chronic irritation. Children may be especially sensitive, and chronic rubbing can increase the risk of infection or worsen inflammation.
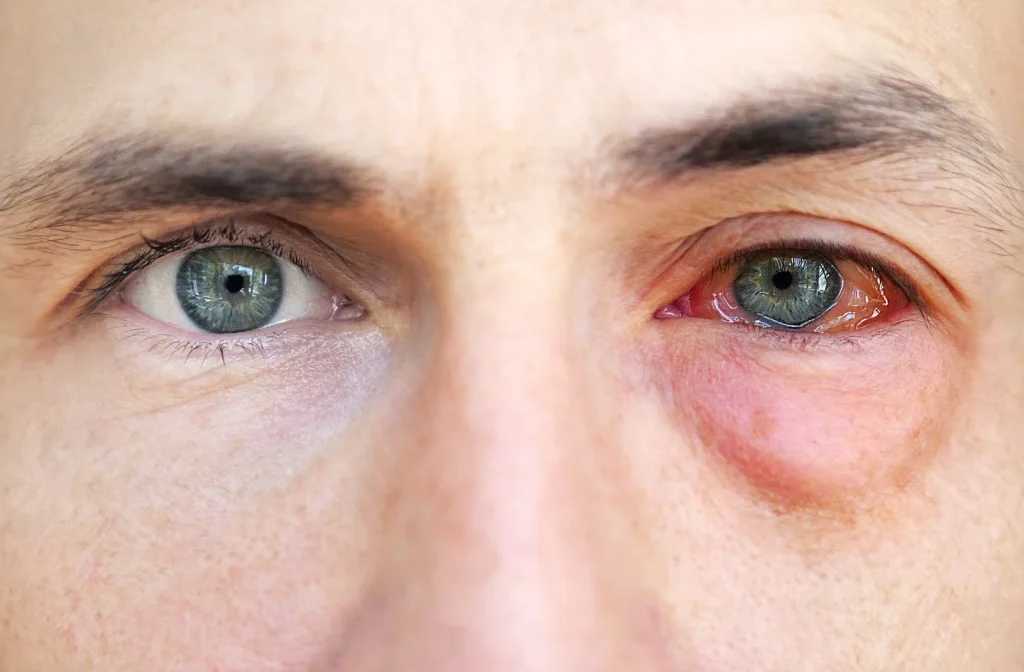
Causes and Risk Factors of Eye Allergies
Eye allergies are influenced by genetic and environmental factors. Common triggers include:
Outdoor Allergens
Pollen from trees, grasses, and weeds
Seasonal variation: spring and fall tend to be peak times
Indoor Allergens
Dust mites in bedding and carpets
Mold in damp areas like basements and bathrooms
Pet dander from cats, dogs, or other animals
Irritants
Cigarette smoke, perfumes, cosmetics, and diesel exhaust
Contact lens residues or reactions to preservatives in drops
Other Factors
High humidity, dry air, or pollution can worsen symptoms
Certain foods or insect bites may trigger eye reactions in sensitive individuals
Risk factors include a family history of allergies, asthma, eczema, or other atopic conditions, as well as prior eye surgeries or chronic contact lens wear.
Types of Eye Allergies
Eye allergies can manifest in different forms, each with unique characteristics:
Seasonal Allergic Conjunctivitis (SAC)
Occurs in spring, summer, or fall
Triggered by pollen
Symptoms: intense itching, redness, tearing, puffy eyelids, light sensitivity
May accompany hay fever, sneezing, or nasal congestion
Perennial Allergic Conjunctivitis (PAC)
Occurs year-round due to indoor allergens like dust mites or pet dander
Usually milder than seasonal allergies but persistent
Vernal Keratoconjunctivitis (VKC)
Chronic, severe allergy, mostly in boys and young men
Symptoms: intense itching, thick mucus, foreign body sensation, photophobia
Associated with eczema or asthma
Untreated VKC can impair vision
Atopic Keratoconjunctivitis (AKC)
Chronic allergy in adults with atopic dermatitis
Symptoms: severe itching, redness, thick mucus, eyelid sticking
Risk of corneal scarring if untreated
Contact Allergic Conjunctivitis
Caused by contact lenses or irritants from solutions
Symptoms: redness, itching, mucus discharge, lens discomfort
Giant Papillary Conjunctivitis (GPC
Severe reaction to contact lenses
Fluid-filled bumps on the eyelids, tearing, blurred vision, poor lens tolerance
Diagnosing Eye Allergies
Accurate diagnosis is essential because eye allergies can mimic infections. Diagnosis may include:
Review of medical history and symptoms
Eye examination with a slit-lamp microscope to detect swollen blood vessels or conjunctival changes
Testing for white blood cells in the conjunctiva via gentle scraping
Identifying allergen triggers through skin or blood tests
Early diagnosis ensures proper treatment and prevents long-term complications like corneal damage.
Managing and Preventing Eye Allergies
Allergen Avoidance
Outdoor Exposure:
Stay indoors during peak pollen times (mid-morning, early evening)
Avoid using window fans that bring in pollen or mold
Wear wraparound sunglasses to protect your eyes
Avoid rubbing your eyes
Indoor Exposure:
Keep windows closed and use air conditioning
Reduce exposure to dust mites with mite-proof bedding covers
Wash bedding in hot water (≥130°F) regularly
Use a dehumidifier to control mold
Clean floors and surfaces with damp mops rather than dry dusting
Pet Allergens:
Wash hands and clothes after pet contact
Keep pets out of bedrooms if allergic
Minimize carpet and furniture that traps dander
Eye Allergy Treatment Options
Effective eye allergy treatment combines lifestyle modifications, over-the-counter solutions, prescription medications, and sometimes advanced therapies.
Over-the-Counter (OTC) Treatments
Artificial tears: wash allergens, relieve dryness, soothe irritation
Decongestant eye drops: reduce redness (short-term use only, max 2–3 days)
Antihistamine drops: relieve itching and redness
Oral antihistamines: reduce allergic response but may dry eyes
Warning: Long-term use of decongestants can worsen redness (rebound effect). Some OTC eye drops may contain preservatives that cause reactions; consider preservative-free options.
Prescription Eye Allergy Drops
Antihistamine drops: quick relief for redness, itching, and swelling
Mast cell stabilizers: prevent histamine release, providing long-term relief
Combination drops: antihistamine + mast cell stabilizer
NSAID drops: reduce inflammation and itching
Corticosteroid drops: for severe inflammation; supervision required
Nonsedating oral antihistamines: reduce itching with fewer sedating effects
Allergy Shots (Immunotherapy)
Gradual exposure to allergens to increase tolerance
Effective for persistent or severe symptoms
Long-term benefits may take months but can significantly reduce symptoms

Understanding Eye Allergy Triggers in Detail
Eye allergies can be triggered by a wide variety of substances. Recognizing your specific triggers is the first step in preventing irritation and minimizing symptoms.
Seasonal Triggers
Tree pollen: Often peaks in early spring, causing flare-ups in March and April.
Grass pollen: Typically highest in late spring and early summer.
Weed pollen: Ragweed pollen is a common culprit in late summer and early fall.
Patients with seasonal allergic conjunctivitis (SAC) often notice symptoms coinciding with these periods, including itching, redness, and tearing. For those with asthma or nasal allergies, these symptoms may worsen during these months.
Indoor Triggers
Indoor allergens can cause perennial allergic conjunctivitis (PAC), which occurs year-round. Common indoor triggers include:
Dust mites: Found in mattresses, pillows, carpets, and upholstered furniture.
Mold spores: Thrive in humid areas such as bathrooms, kitchens, and basements.
Pet dander: Cats, dogs, birds, and small mammals shed skin cells that can trigger allergic reactions.
Minimizing exposure to indoor triggers requires careful attention to cleaning routines, air filtration, and humidity control.
Irritants and Chemical Triggers
Smoke: Cigarette smoke or wildfire smoke can aggravate symptoms.
Perfumes and scented products: Fragrances in personal care products, air fresheners, or cleaning agents may trigger eye redness and irritation.
Preservatives in eye drops or cosmetics: Certain chemicals in lubricating drops or makeup can provoke allergic reactions. Using preservative-free or hypoallergenic products is often safer.
Other Triggers
Although less common, some people may react to:
Foods or food additives (rarely)
Insect bites or stings
Environmental pollutants like diesel exhaust or industrial fumes
By keeping a symptom diary, you can identify patterns and triggers, making it easier to avoid them or adjust treatments accordingly.
Lifestyle and Home Strategies for Prevention
Prevention is as important as treatment in managing eye allergies. Practical lifestyle adjustments can dramatically reduce symptoms:
Home Environment
Maintain low humidity: Use dehumidifiers in basements or damp rooms to prevent mold growth.
Keep bedding allergen-free: Wash sheets, pillowcases, and blankets in hot water (≥130°F) weekly. Use dust-mite-proof covers for pillows, mattresses, and comforters.
Clean smartly: Damp mop floors instead of dry dusting to trap dust and allergens. Vacuum with a HEPA filter vacuum.
Air filtration: Use HEPA filters in air conditioners or standalone air purifiers. Clean units regularly to avoid circulating allergens.
Personal Habits
Hand hygiene: Wash hands after touching pets, cleaning, or gardening.
Avoid eye rubbing: Rubbing spreads allergens and can worsen inflammation.
Protective eyewear: Wear sunglasses or wraparound glasses outdoors during high-pollen days or windy conditions.
Travel and Outdoor Considerations
Monitor local pollen counts via online apps or weather reports.
Plan outdoor activities when pollen levels are lower, usually late morning or after rain.
Shower and change clothes after outdoor exposure to remove pollen from skin and hair.
Eye Allergies in Special Situations
Contact Lens Wearers
Lens discomfort or redness may indicate contact allergic conjunctivitis or giant papillary conjunctivitis.
Using daily disposable lenses, cleaning solutions with fewer preservatives, or taking breaks from lenses can help.
Children
Symptoms may include eye rubbing, eyelid swelling, and tearing.
Artificial tears and certain antihistamine drops are safe for children 3+ years.
Persistent symptoms require pediatric allergist evaluation.
Elderly
Aging eyes may be drier, making eye allergies more uncomfortable.
Use of preservative-free drops and careful medication selection is essential.
Coexisting Eye Conditions
Patients with glaucoma or cataracts must avoid certain decongestant or steroid drops unless prescribed.
Eye allergy symptoms may mimic infections or other eye diseases, emphasizing the need for professional diagnosis.
Potential Complications if Untreated
Chronic eye rubbing can cause corneal scratches or infections.
Severe allergies like VKC or AKC can scar the cornea, potentially impairing vision.
Persistent inflammation may increase sensitivity to light and interfere with daily activities.
Secondary eye infections can occur if mucus and discharge are not managed.
Eye Allergy Treatment for Children
Children can safely use eye allergy drops and medications under a doctor’s supervision. Artificial tears are safe for all ages, while antihistamine and mast cell stabilizer drops are typically approved for children 3 years and older. Consult a pediatric allergist to design a safe, age-appropriate treatment plan.
Long-Term Prevention Strategies
Chronic eye allergies can cause serious eye damage if left untreated, including corneal scarring. Long-term prevention involves:
Avoiding allergens whenever possible
Maintaining clean indoor environments
Using prescribed eye allergy drops regularly
Wearing protective eyewear outdoors
Following up with an allergist to monitor eye health
Adhering to these strategies reduces the risk of complications and helps maintain clear vision.
When to See an Allergist or Eye Specialist
Seek professional care if:
Over-the-counter eye allergy drops don’t relieve symptoms
You experience severe itching, redness, or swelling
Vision is blurred or affected
Symptoms persist year-round despite home management
An allergist can provide accurate diagnosis, prescribe effective medications, and develop a long-term management plan for your eye allergy treatment.
Great External Resources
Frequently Asked Questions (FAQs)
What causes eye allergies?
They occur when your immune system overreacts to harmless substances called allergens, such as pollen, dust mites, pet dander, mold, or smoke. The eyes release histamine and other chemicals in response, causing redness, itching, swelling, and tearing.
What are the common symptoms of eye allergies?
Symptoms include itchy eyes, redness, watery eyes, burning or stinging, swollen eyelids, sensitivity to light, and a feeling that something is in your eye. Some people may also experience nasal congestion or sneezing alongside eye symptoms.
Can eye allergies cause blurry vision?
Yes, they can cause temporary blurry vision. This usually happens due to excessive tearing, swelling of the conjunctiva, or rubbing the eyes. Blurry vision from eye allergies is generally mild and resolves once the allergy is treated.
Can eye allergies cause headaches?
They can indirectly trigger headaches. Sinus congestion, sinus pressure, or eye strain from rubbing itchy eyes can contribute to mild to moderate headaches. Treating the allergy often helps reduce these headaches.
Can eye allergies cause blindness?
Eye allergies themselves are not likely to cause blindness. However, severe chronic allergic conditions—like vernal keratoconjunctivitis or atopic keratoconjunctivitis—can lead to corneal damage if untreated, which could affect vision. Prompt treatment prevents serious complications.
Can eye allergies be cured?
There is no permanent “cure” for eye allergies, but they can be effectively managed. Avoiding triggers, using antihistamine or mast cell stabilizer eye drops, and following prescribed treatments can control symptoms and improve quality of life.
Can eye allergies cause eye pain?
Yes, eye allergies can cause mild to moderate discomfort or burning sensations. Severe allergic reactions may also lead to soreness from constant rubbing or swelling of the eyelids.
Can eye allergies affect only one eye?
While eye allergies often affect both eyes, it is possible for symptoms to appear in just one eye, especially if only one eye is exposed to the allergen or if contact lenses are involved.
Can eye allergies cause a runny nose?
Yes, eye allergies are frequently part of a larger allergic response that includes nasal symptoms like a runny or stuffy nose, sneezing, and postnasal drip. This is commonly seen in allergic rhinitis or rhinoconjunctivitis.
Can eye allergies cause floaters?
Eye allergies do not typically cause floaters. Floaters are usually related to changes in the vitreous gel inside the eye or retinal issues. If floaters appear suddenly or are accompanied by flashes of light, it’s important to see an eye specialist.