What are Cataracts?
A cataract is the clouding of the natural lens of the eye, which lies behind the iris and pupil. It develops gradually over time, often leading to blurred or cloudy vision. In its early stages, cataracts may not cause noticeable vision impairment, but over time, the cloudiness becomes denser, blocking more light from entering the eye. As the cataract progresses, it can severely impair vision and make everyday activities like reading, driving, and even recognizing faces difficult.
Cataracts are generally associated with aging, affecting many people over the age of 55. However, they can also occur in younger people due to genetic factors, trauma, certain medications (e.g., steroids), or systemic diseases like diabetes. Cataracts can develop in one or both eyes and often result in symptoms such as:
Blurry or cloudy vision
Difficulty seeing at night or in low-light conditions (night blindness)
Sensitivity to light or glare
Faded or yellowed colors
Frequent changes in eyeglass prescriptions
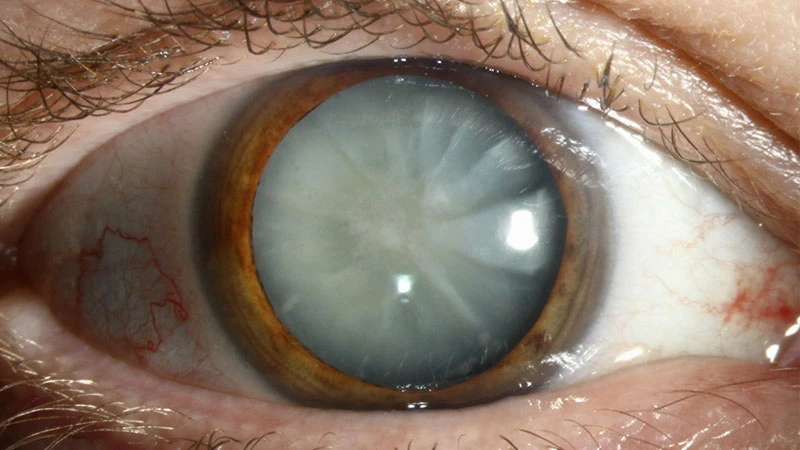
Common Causes of Cataracts
Cataracts are most commonly caused by the aging process, but several factors can accelerate their development, including:
Age: The most common cause of cataracts is age. As we get older, the proteins in the eye’s lens naturally break down, causing the lens to become cloudy.
Diabetes: People with diabetes are at a higher risk of developing cataracts, as high blood sugar levels can affect the lens of the eye.
UV Radiation: Prolonged exposure to ultraviolet (UV) light, either from the sun or artificial sources, can increase the likelihood of developing cataracts.
Smoking: Smoking increases the risk of cataract formation because of the chemicals in cigarettes that damage the lens.
Eye Injury: Trauma to the eye can cause cataracts, either immediately or years later.
Genetics: Family history plays a role in determining susceptibility to cataracts, especially when they occur at a young age.
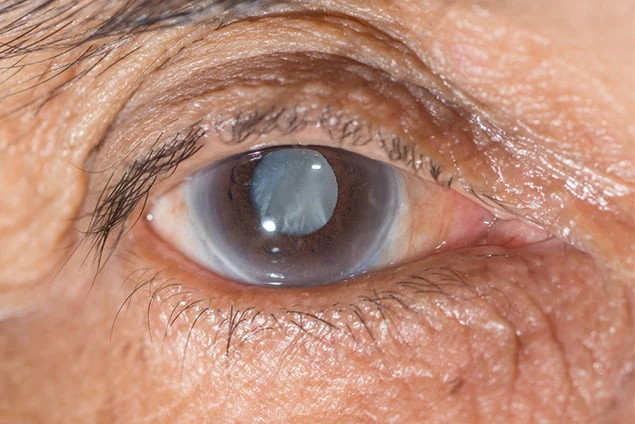
Types of Cataracts
Cataracts are classified into three main types based on their location in the lens:
Nuclear Cataract
Location: This type of cataract forms in the nucleus, the central part of the lens.
Symptoms: Nuclear cataracts typically develop slowly, causing gradual vision changes. The primary symptom is blurred or cloudy vision, often accompanied by yellowing of colors.
Cause: They are commonly associated with the natural aging process.
Cortical Cataract
Location: This cataract forms in the cortex, the outer region of the lens, and develops as spoke-like opacities that extend from the edge of the lens toward the center.
Symptoms: Symptoms may include glare, sensitivity to light, and difficulty seeing at night.
Cause: Cortical cataracts are often linked to diabetes and other metabolic conditions.
Subcapsular Cataract
Location: Subcapsular cataracts develop at the back of the lens, just beneath the lens capsule.
Symptoms: This type of cataract can cause problems with reading, glare, and difficulty seeing in bright light.
Cause: These cataracts are frequently seen in people with diabetes, those taking steroid medications, or individuals with high myopia (nearsightedness).
In some cases, cataracts can also be congenital, meaning they are present at birth or develop shortly after birth. These rare cataracts are often caused by genetic conditions, infections during pregnancy, or other factors.
How Is Cataract Eye Surgery Performed?
Cataract surgery is a safe, routine procedure that removes the cloudy lens and replaces it with an artificial lens (Intraocular Lens, or IOL). The surgery is typically performed on an outpatient basis, meaning you can go home the same day after the procedure. Here’s an overview of how the procedure works:
Step 1: Preoperative Assessment
Before surgery, a comprehensive eye exam is conducted to assess the type and severity of the cataract. This includes measuring the curvature of the cornea, eye length, and other factors to determine the appropriate type of IOL for you.
Step 2: Anesthesia
Cataract surgery is usually done under local anesthesia, which numbs the eye but keeps you awake. Some patients may also receive a mild sedative to help them relax.
Step 3: Incision and Lens Removal
A small incision is made on the surface of the eye, and a tiny probe is inserted. For Phacoemulsification, this probe emits ultrasonic waves to break up the cloudy lens, which is then gently suctioned out of the eye.
Step 4: IOL Implantation
Once the cloudy lens is removed, a clear, artificial IOL is inserted. The IOL is carefully positioned in the eye where the natural lens used to be. There are different types of IOLs, including monofocal, multifocal, and toric IOLs, which are selected based on your visual needs and preferences.
Step 5: Recovery and Aftercare
After the surgery, you will be given eye drops to prevent infection and reduce inflammation. The eye is usually covered with a protective shield or bandage, which you should wear for a period of time. Postoperative care also includes follow-up appointments to monitor healing and ensure that the IOL is correctly positioned.
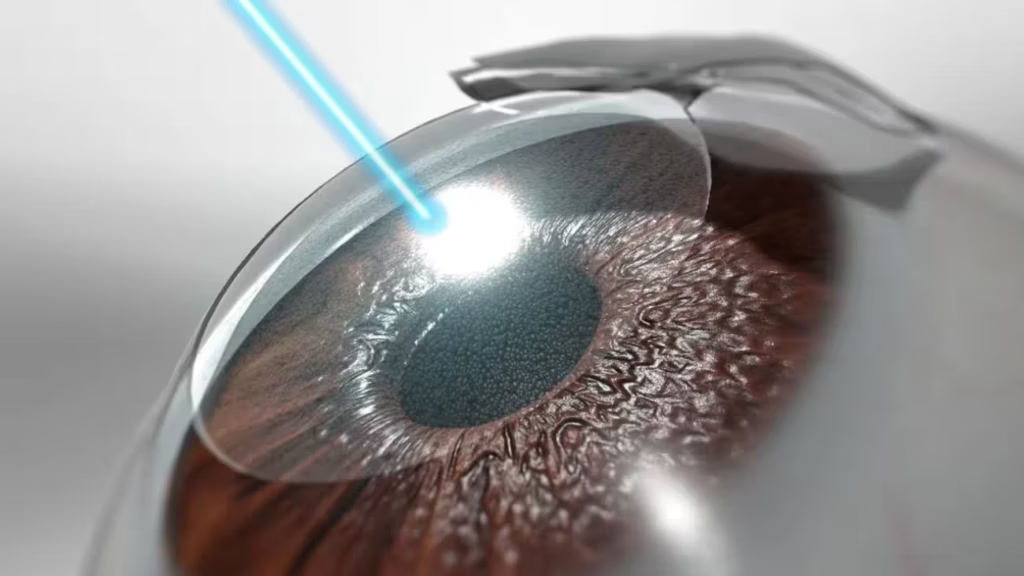
Surgical Alternatives: Femtosecond Laser-Assisted Cataract Surgery
An advanced alternative to traditional cataract surgery is femtosecond laser-assisted cataract surgery. This technique uses a laser to make precise incisions and break up the cataract, offering more accuracy, less discomfort, and quicker recovery times. At Ebsaar, we offer the latest technology to give patients the best possible outcomes.

Cataract Surgery Recovery
Cataract surgery has one of the highest success rates in medical procedures, with around 90% of patients experiencing improved vision post-surgery. While recovery times vary, most patients can resume normal activities, such as reading and watching TV, within a few days. However, some precautions should be taken during the healing process:
Avoid Eye Strain: Refrain from heavy lifting, strenuous exercise, and activities that strain the eyes.
Use Medications: Take prescribed antibiotic and anti-inflammatory drops as directed.
Protect Your Eyes: Wear sunglasses to protect your eyes from UV light and avoid rubbing your eyes during recovery.
Follow-up Appointments: Regular checkups are essential to monitor your recovery and address any complications, though these are rare.
Potential Risks and Complications
While cataract surgery is generally safe, like all surgeries, it carries some risks. Potential complications can include infection, inflammation, elevated intraocular pressure, or changes in the IOL’s position. However, these risks are minimized with proper care, and most patients recover without major issues.
Great External Resources
Frequently Asked Questions (FAQs)
When to do eye cataract surgery?
It is typically recommended when cataracts significantly affect your vision and interfere with daily activities, such as reading, driving, or watching TV. If cataracts cause blurred vision, glare, or night blindness that cannot be corrected with glasses or other treatments, it’s time to consider surgery. The decision is usually made in consultation with an eye specialist who will evaluate the severity of the cataract and its impact on your quality of life.
When was the first cataract eye surgery?
The first documented surgery dates back over 2,000 years to ancient India. The procedure, known as “couching”, involved using a needle to dislodge the cataract and push it to the back of the eye. In modern times, Phacoemulsification, developed in the 1960s by Dr. Charles Kelman, revolutionized cataract surgery, making it safer, more effective, and minimally invasive.
What is cataract eye surgery?
It is a medical procedure used to remove the cloudy lens in the eye caused by cataracts. The cloudy lens is replaced with an artificial intraocular lens (IOL), restoring clear vision. The surgery is typically quick, minimally invasive, and is performed on an outpatient basis, meaning the patient can go home the same day.
How long is the recovery from cataract eye surgery?
The recovery is relatively quick for most patients. Initial healing can take anywhere from 1-2 weeks, during which you may need to avoid strenuous activities and follow your doctor’s instructions closely. Full recovery, including stabilization of vision, may take 4-6 weeks. During this time, follow-up appointments will be scheduled to monitor the healing process and ensure everything is progressing as expected.
How cataract eye surgery is done?
It is typically performed under local anesthesia. The surgeon makes a small incision in the cornea, then uses an ultrasound probe to break up and remove the cloudy lens (a process called phacoemulsification). Afterward, an artificial lens (intraocular lens, or IOL) is implanted to replace the natural lens. The incision is usually so small that stitches are not required. The entire procedure typically lasts less than an hour.
How safe is cataract eye surgery?
It is generally very safe, with a success rate of about 90-95%. Complications are rare but can include infection, inflammation, or increased eye pressure. The risk of complications can be minimized by following post-surgery care instructions and attending follow-up appointments. Cataract surgery has one of the highest success rates in surgery, and most patients experience a significant improvement in their vision.
How long is cataract eye surgery?
It typically takes 15-30 minutes. It is performed on an outpatient basis, meaning you can usually return home the same day. The procedure itself is quick and minimally invasive, and most patients experience little to no discomfort during surgery.
Can dogs have cataract eye surgery?
Yes, dogs can undergo surgery. We don’t offer this service however. Cataract surgery for dogs is similar to human cataract surgery and involves the removal of the cloudy lens and its replacement with an artificial lens (IOL). However, the procedure is more complex in animals, and the success rate can vary depending on the dog’s age, health, and the severity of the cataracts. It’s essential to consult with a veterinary ophthalmologist to determine the best course of action for your pet.
Why is the eye blurry after cataract surgery?
Blurry vision after the procedure is common and can happen for several reasons, including:
Post-surgery healing: It may take a few days to weeks for your eye to fully heal.
Intraocular lens (IOL) adjustment: It may take some time for the brain to adjust to the new IOL, especially if it’s a multifocal or toric lens.
Dry eyes: Cataract surgery can temporarily affect the tear film, leading to blurry vision. Dry eye symptoms should improve as healing progresses.
Other eye conditions: Occasionally, conditions like macular edema or glaucoma may cause temporary blurriness after surgery.
If blurry vision persists or worsens, it’s important to contact your eye doctor for a follow-up exam.
Why does cataract surgery cause dry eye?
Surgery can cause temporary dry eye symptoms due to several factors:
Disruption of the tear film: The surgery can temporarily affect the production of tears or the stability of the tear film, leading to dryness.
Anesthesia: The use of local anesthesia and eye drops during the surgery can reduce blinking and tear production temporarily.
Healing process: As your eye heals from the surgery, dry eye symptoms may occur, but they usually improve within a few weeks.
Your doctor may recommend lubricating eye drops to help manage dry eye symptoms during the recovery period.
Why wear an eye patch after cataract surgery?
An eye patch is typically recommended after surgery to protect the eye during the initial healing phase. The patch helps prevent accidental rubbing or pressure on the eye while it is healing and reduces the risk of infection. It also helps minimize discomfort and shields the eye from bright light or dust. Your doctor will provide instructions on how long to wear the patch, usually for a few hours after the surgery or overnight for the first few days.
Why cataract surgery only one eye at a time?
It is generally performed on one eye at a time to reduce the risks associated with operating on both eyes simultaneously. This allows the surgeon to monitor the healing process and ensure the best possible outcome for the first eye before proceeding with surgery on the other eye. In most cases, surgery for the second eye is scheduled several weeks after the first to give the first eye time to heal properly. This approach minimizes complications and ensures better overall recovery.