Quick Links
- What is Macular Degeneration?
- Who is at Risk for Macular Degeneration?
- Symptoms of Macular Degeneration
- Diagnosis of Macular Degeneration
- Advanced Macular Degeneration Treatment Options
- Living With Macular Degeneration
- Prevention and Risk Reduction
- Great External Resources
- Frequently Asked Questions (FAQs)
What is Macular Degeneration?
Macular degeneration, sometimes called age-related macular degeneration (AMD), is an eye condition affecting the central retina, called the macula. The macula is responsible for sharp, detailed central vision, which allows you to read, drive, and recognize faces.
There are two primary types of macular degeneration:
Dry (Atrophic) Macular Degeneration:
Dry AMD is the most common form, accounting for approximately 80–90% of cases. It develops gradually when tiny protein deposits called drusen accumulate under the macula, leading to thinning and weakening of this critical tissue. Vision loss is slow, but over time, it can affect daily tasks significantly.Wet (Exudative) Macular Degeneration:
Wet AMD is less common but more severe. It occurs when abnormal blood vessels grow under the retina and macula, leaking fluid and blood. This can lead to rapid central vision loss, dark spots, or distortion in the vision. Wet AMD often develops suddenly and requires immediate medical attention.
Both types of macular degeneration affect the quality of life but differ in their progression, treatment, and prognosis.
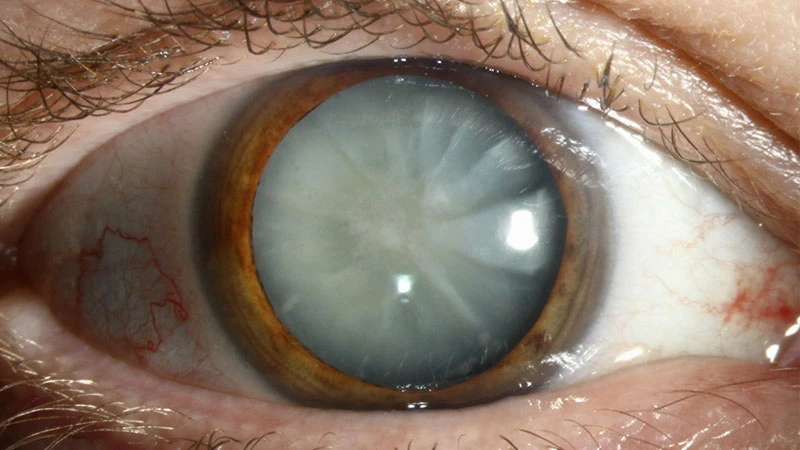
Who is at Risk for Macular Degeneration?
While macular degeneration is primarily age-related, several factors can increase your risk:
Age: Most cases occur in adults over 50.
Family History: Genetics play a role; if close relatives have AMD, your risk is higher.
Lifestyle Factors: Smoking, high blood pressure, obesity, and diets high in saturated fats can contribute to AMD.
Ethnicity: Caucasians are at higher risk of developing AMD compared to other ethnic groups.
Other Health Conditions: Diabetes, cardiovascular disease, and previous eye injuries can increase susceptibility.
Understanding these risk factors allows your ophthalmologist to create a tailored monitoring and treatment plan to protect your vision.
Symptoms of Macular Degeneration
Macular degeneration primarily affects central vision. Common symptoms include:
Blurred or Wavy Vision: Straight lines may appear distorted or bent.
Dark or Blank Spots: Central vision may have shadowed areas.
Difficulty Seeing in Low Light: Tasks like reading at night become challenging.
Changes in Color Perception: Colors may appear duller or less vibrant.
Gradual or Sudden Vision Loss: Depending on whether you have dry or wet AMD.
Early detection is critical. If you notice any changes in your central vision, consult a retinal specialist promptly to explore macular degeneration treatment options.
Diagnosis of Macular Degeneration
Detecting AMD in its early stages significantly improves treatment outcomes. A comprehensive eye exam can determine the type and severity of macular degeneration. Key diagnostic tests include:
Amsler Grid Test: Detects vision distortions and wavy lines, a hallmark of AMD.
Dilated Eye Exam: Eye drops are used to widen your pupils, allowing your ophthalmologist to examine the retina and macula.
Optical Coherence Tomography (OCT): Provides detailed cross-sectional images of the retina, revealing early signs of degeneration.
Fluorescein Angiography: Highlights leaking blood vessels in wet AMD using a special dye.
OCT Angiography (OCTA): Non-invasive imaging of blood flow in the retina to detect abnormal vessels.
Accurate diagnosis ensures the right macular degeneration treatment plan is prescribed for your unique condition.
Advanced Macular Degeneration Treatment Options
There is no cure for macular degeneration, but modern treatments can slow disease progression, preserve central vision, and enhance quality of life. The treatment approach depends on whether the AMD is dry or wet.
Treatments for Dry Macular Degeneration
While dry AMD cannot be reversed, certain interventions can slow its progression:
Nutritional Supplements (AREDS2 Formula):
A combination of vitamins and minerals — including Vitamin C, Vitamin E, zinc, copper, lutein, and zeaxanthin — has been shown to reduce the risk of progression in intermediate-stage AMD.Lifestyle Adjustments:
Quit smoking.
Maintain a healthy diet rich in leafy greens, fish, and antioxidants.
Manage blood pressure and cholesterol.
Exercise regularly.
Low Vision Support:
Magnifying glasses, special lighting, and digital aids can help patients maintain independence despite central vision loss.
Treatments for Wet Macular Degeneration
Wet AMD requires more active intervention due to rapid vision loss. Available treatments include:
Anti-VEGF Injections:
Drugs such as Aflibercept (Eylea®), Ranibizumab (Lucentis®), Bevacizumab (Avastin®), and Faricimab (Vabysmo®) are injected into the eye to block VEGF protein and stop abnormal blood vessel growth. Regular treatments help maintain and sometimes improve vision.Photodynamic Therapy (PDT):
Combines a light-sensitive drug with a laser to destroy leaky blood vessels while preserving surrounding healthy tissue.Laser Photocoagulation:
Seals off leaking blood vessels, preventing further vision loss.Gene Therapy (Emerging Treatment):
Investigational gene therapies aim to reduce the need for repeated injections by enabling the eye to produce its own anti-VEGF medication.Stem Cell Therapy (Experimental):
Stem cells may one day replace damaged retinal cells in late-stage dry AMD, offering hope for vision restoration.
Living With Macular Degeneration
Adjusting to life with AMD can be challenging. Some tips to maintain independence include:
Use magnifiers or digital reading aids.
Ensure adequate lighting in your home.
Arrange your workspace to reduce eye strain.
Regularly monitor vision changes using an Amsler grid.
Seek emotional support; AMD can cause anxiety or depression due to vision loss.
Support groups and rehabilitation programs can help patients adapt to daily activities while living with macular degeneration.

Prevention and Risk Reduction
While age and genetics cannot be changed, lifestyle modifications can reduce your risk:
Stop smoking.
Maintain a balanced diet with antioxidants, leafy greens, and omega-3 fatty acids.
Control blood pressure and cholesterol.
Exercise regularly to improve blood flow to the eyes.
Schedule regular eye exams to catch AMD early.
Early intervention allows for timely macular degeneration treatment that can slow or prevent severe vision loss.
Great External Resources
Frequently Asked Questions (FAQs)
Can macular degeneration cause blindness?
Macular degeneration primarily affects the central part of your vision, so complete blindness is rare. Most people retain their peripheral vision, which allows them to navigate spaces and detect objects around them. However, central vision loss can make reading, recognizing faces, and performing daily tasks very difficult. Wet macular degeneration progresses more rapidly and can lead to severe central vision impairment if untreated.
Early detection and treatment, such as anti-VEGF injections for wet AMD or AREDS2 supplements for dry AMD, can significantly slow vision loss. While you may not lose all vision, untreated macular degeneration can drastically affect quality of life, making it essential to schedule regular eye exams and consult a retinal specialist at the first sign of symptoms. Maintaining a healthy lifestyle and following your eye care provider’s guidance can also help preserve vision for as long as possible.
Will macular degeneration always get worse over time?
Macular degeneration is generally a progressive condition, but its rate of progression varies widely between individuals. Dry AMD usually develops slowly, often over many years, while wet AMD can worsen quickly. Not everyone will experience severe vision loss, and some people may live for decades with minimal impact on their daily lives. Risk factors such as smoking, poor diet, and high blood pressure can accelerate progression, whereas lifestyle modifications and early treatment can slow it down.
Monitoring your vision through regular eye exams, Amsler grid tests at home, and following a retinal specialist’s recommendations can help manage disease progression. Treatments, such as anti-VEGF injections for wet AMD, can stabilize vision, while AREDS2 nutritional supplements can slow the progression of intermediate dry AMD. Early detection is key to slowing or even halting further damage.
Is there a cure for macular degeneration?
Currently, there is no cure for macular degeneration. The condition damages the macula, which is central to detailed vision, and this damage is generally irreversible. However, modern treatments can significantly slow disease progression, stabilize vision, and improve quality of life. For dry AMD, AREDS2 nutritional supplements have been proven to reduce the risk of vision loss.
Wet AMD can be treated with anti-VEGF injections, photodynamic therapy, and laser treatments to prevent rapid central vision loss. Emerging therapies like gene therapy and stem cell transplantation hold promise for the future, potentially offering ways to restore some vision or reduce the need for repeated injections. Even without a cure, early detection and consistent management allow many patients to retain their vision for years, maintaining independence and daily functioning.
What causes macular degeneration?
Macular degeneration occurs when the macula, the central part of the retina responsible for sharp vision, begins to deteriorate. Age is the most significant risk factor, which is why it’s commonly referred to as age-related macular degeneration (AMD). Genetics also play a role; having family members with AMD increases your likelihood of developing the condition.
Other contributors include smoking, poor nutrition, high blood pressure, obesity, and chronic inflammation in the eyes. In dry AMD, tiny deposits called drusen accumulate under the retina, causing thinning and weakening. In wet AMD, abnormal blood vessels grow under the macula, leaking fluid and blood, which can rapidly damage vision. Understanding these causes helps patients adopt preventive measures, such as quitting smoking, eating an antioxidant-rich diet, controlling blood pressure, and having regular eye exams to detect early signs of macular degeneration.
Why does macular degeneration cause visual hallucinations?
Visual hallucinations in macular degeneration, known as Charles Bonnet Syndrome, occur when the brain compensates for vision loss. As central vision deteriorates, the brain receives incomplete visual input from the retina, leading it to create images that appear real. These hallucinations are usually harmless and can include patterns, shapes, or even detailed images of people or objects.
They are more common in older adults with significant central vision loss but are not a sign of mental illness. While the exact cause is not fully understood, it is believed to be a neurological response to the lack of visual stimulation. Patients experiencing these hallucinations should inform their ophthalmologist, as supportive counseling and education can reduce anxiety and help them manage the episodes effectively. Understanding this phenomenon reassures patients that the hallucinations are a normal reaction to vision loss.
Where in the eye does macular degeneration begin?
Macular degeneration begins in the macula, which is the small, central area of the retina located at the back of the eye. The macula is responsible for sharp, detailed central vision, allowing tasks like reading, driving, and recognizing faces. In dry AMD, the earliest changes are often tiny yellow deposits called drusen that accumulate under the macula, gradually thinning the retinal tissue. In wet AMD, abnormal blood vessels develop underneath the macula, causing fluid leakage and rapid distortion of central vision.
Peripheral vision remains largely unaffected because macular degeneration primarily targets this central area. Early detection of changes in the macula through routine eye exams, OCT imaging, or Amsler grid tests allows for timely intervention and slows disease progression.
At what age does macular degeneration typically start?
Macular degeneration most commonly affects adults over the age of 50, which is why it’s often called age-related macular degeneration (AMD). However, younger adults can occasionally develop the condition due to genetic factors, previous eye injuries, or underlying medical conditions such as diabetes. Early-stage macular degeneration may not cause noticeable symptoms, which is why regular eye exams are critical for adults starting in their 50s.
Risk increases with age, and the likelihood of developing wet AMD is higher in later stages. Lifestyle choices, including smoking and poor nutrition, can accelerate onset and progression. Monitoring your eyes regularly and maintaining a healthy lifestyle can help detect early changes and allow prompt initiation of macular degeneration treatment before significant vision loss occurs.
When should I be tested for macular degeneration?
Testing for macular degeneration should begin around age 50, especially if you have risk factors such as a family history of AMD, smoking, high blood pressure, or obesity. Even if you have no symptoms, routine eye exams can detect early changes in the macula. Tests may include a dilated eye exam, OCT imaging, and Amsler grid testing, which reveal thinning, drusen deposits, or abnormal blood vessels.
If you notice changes in vision, such as blurry spots, wavy lines, or difficulty reading, you should see a retinal specialist immediately, regardless of age. Early detection is crucial because interventions like nutritional supplements for dry AMD or anti-VEGF injections for wet AMD are most effective before significant vision loss occurs. Regular monitoring ensures timely macular degeneration treatment to preserve central vision.
What does macular degeneration look like in vision?
Macular degeneration affects the central part of your vision, often causing blurred or wavy images. Straight lines may appear distorted, and dark or blank spots can form in the center of your visual field. Colors may look duller or less vibrant, and reading or recognizing faces becomes challenging. Peripheral vision usually remains intact, so you can still see objects on the sides.
People with wet AMD may notice rapid changes in central vision due to leaking blood vessels, while dry AMD progresses more gradually. Some patients describe the effect as looking through a foggy or blurred area in the middle of their vision. Regular eye exams, OCT imaging, and Amsler grid tests can detect these changes early, allowing ophthalmologists to recommend appropriate macular degeneration treatment to preserve vision.
What does it mean to have macular degeneration?
Having macular degeneration means that the central part of your retina, the macula, is deteriorating. This central vision loss affects tasks requiring fine detail, such as reading, recognizing faces, and driving. While peripheral vision remains mostly unaffected, the impact on daily life can be significant. The condition can be slow-progressing (dry AMD) or rapid (wet AMD), and the severity varies among individuals.
It is considered a chronic eye disease with no cure, but treatments and lifestyle modifications can slow progression and preserve functional vision. Being diagnosed with AMD means you should work closely with an ophthalmologist to monitor your vision, implement preventive strategies, and explore treatments such as nutritional supplements, anti-VEGF injections, or photodynamic therapy, depending on the type of macular degeneration.
Can macular degeneration be reversed?
Currently, macular degeneration cannot be reversed. Damage to the macula is generally permanent, and lost central vision cannot fully return. However, interventions can slow progression, preserve existing vision, and, in some cases, partially improve function. For dry AMD, nutritional supplements like AREDS2 may reduce the risk of further vision loss. Wet AMD can be treated with anti-VEGF injections, which may stabilize vision and sometimes restore a small amount of lost sight.
Experimental treatments, including gene therapy and stem cell transplants, are being researched to repair or replace damaged retinal tissue, but these are not widely available yet. Early detection and consistent management remain the most effective strategies to protect your eyesight and maintain independence.
Can macular degeneration be cured?
At present, there is no cure for macular degeneration. The condition damages the macula, which is essential for central vision, and this damage cannot be fully reversed. Treatments focus on slowing disease progression and preserving vision. For dry AMD, AREDS2 supplements may reduce the risk of worsening vision, while wet AMD can be treated with anti-VEGF injections, laser therapy, or photodynamic therapy.
Emerging therapies such as gene therapy aim to reduce treatment frequency and potentially restore some retinal function, but a full cure is not yet available. Patients can maintain independence and quality of life through early detection, lifestyle modifications, and timely medical interventions. Regular eye exams are essential to detect changes before significant vision loss occurs.
Can macular degeneration be hereditary?
Yes, macular degeneration can run in families. Genetics is one of the major risk factors for developing AMD. Having a parent or sibling with macular degeneration increases your likelihood of developing the condition, particularly if multiple family members are affected. Specific gene variants have been linked to higher susceptibility, and researchers continue to study the hereditary patterns of AMD.
However, lifestyle factors like smoking, poor diet, obesity, and high blood pressure also play a crucial role in disease onset and progression. Even if macular degeneration is hereditary, preventive measures, early detection, and timely treatment can help slow vision loss and improve outcomes. Regular eye exams and discussing family history with your ophthalmologist are key to managing risk.